Pregnancy
Understanding the contraception crisis
How the one-size-fits-all approach fails women and why it has to change
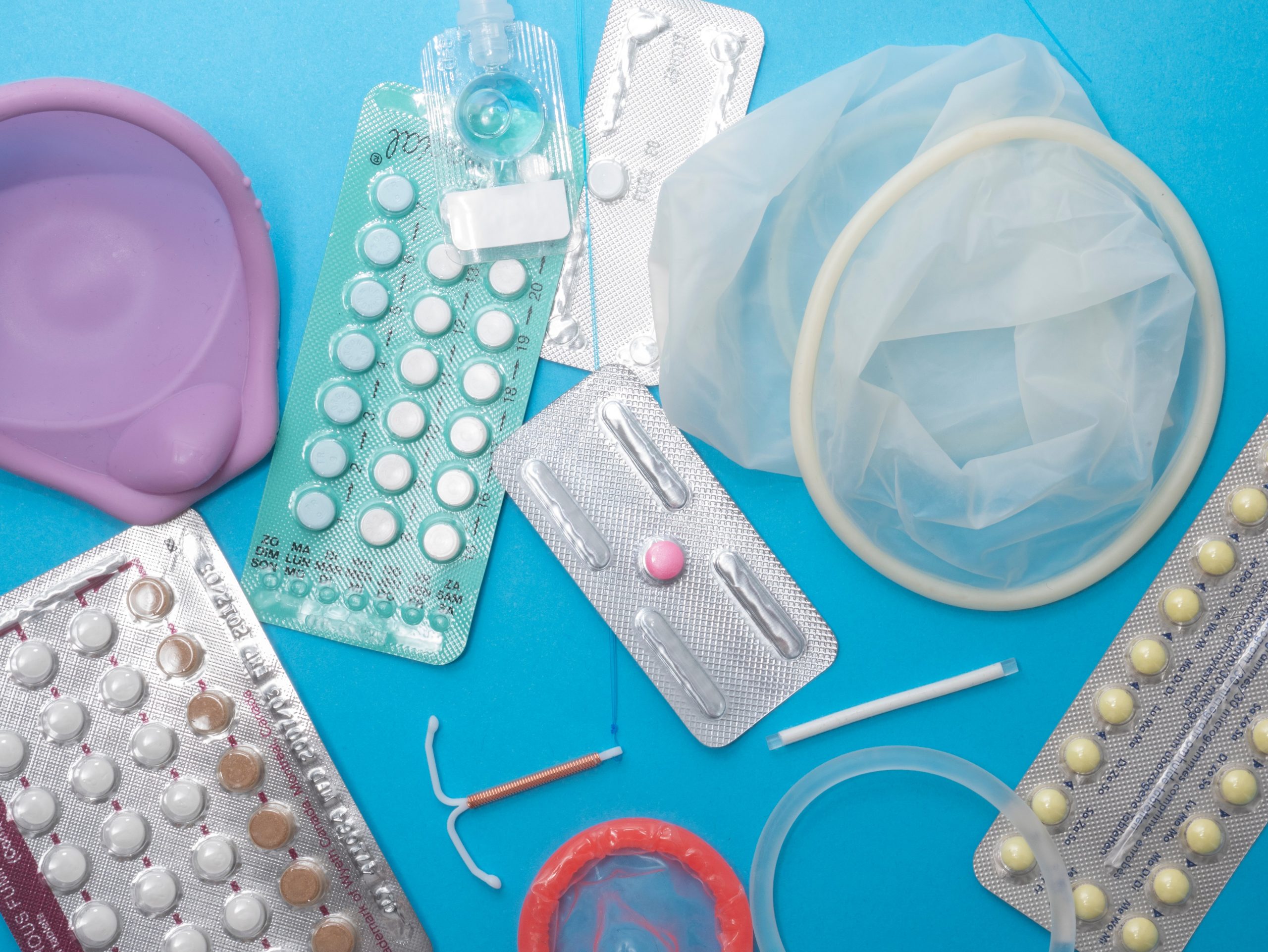
Finding the right contraception method shouldn’t be trial and error, says Elena Rueda Carrasco. She tells FemTech World why understanding contraception is more important than ever.
“Despite encouraging research, a male birth control pill remains elusive,” reads a recent headline in The New York Times.
Although, according to the article, scientists have been researching ways to create a male birth control pill since the 1970s, negative side effects, such as weight gain, acne, irritability and mood swings, have been responsible for not licensing any products for use.
“A woman can struggle with the same symptoms in silence – something rather normalised in our society,” says Elena Rueda Carrasco, medical scientist and co-founder and CEO of Dama Health, a company that offers personalised contraception recommendation. “Many women are being told from a very young age that the pain they are experiencing is normal,” she adds.
Indeed birth control side effects, such as weight gain, mood changes and headaches, affect eight in ten women, but are yet deemed too dangerous for developing a pill for men.
“The side effects and the impact of different contraception methods on women have been very normalised when you compare it to other areas of medicine,” Rueda explains. “In a lot of cases, women end up with conditions like endometriosis and PCOS – polycystic ovary syndrome – because their symptoms are often ignored and early diagnosis is not achieved.”

Elena Rueda Carrasco, co-founder and CEO of Dama Health
Figures suggest that medical consultations are too short to offer the right guidance and on average, women try 3.5 different contraceptive methods before finding the one that works for them.
“In the UK, we have such a fragmented [health] system,” the co-founder says. “As a woman, you can get your contraception through your GP, you can go to a sexual health clinic, you can speak to a nurse or a pharmacist. And from our own research, we found out that for many women, this is very confusing.
“Most of the time women will probably call or visit their GP and the GP is actually not a specialist,” Rueda points out. “The GPs are doing a bit of everything, with just a couple of contraception methods they’re comfortable prescribing. Therefore, communication is really hard when you have this fragmentation happening and you don’t really know where to go and who to speak to”.
Dama Health aims to personalise and tailor the way women are being prescribed contraception, screening for and identifying the side effects that women might experience individually. An algorithm would then match them to the recommended contraceptive options that are most suitable for them.
“As a team, we are all scientists and doctors by background, and we were all experiencing this problem of trial and error in the way that women were being prescribed hormonal medication and in this specific case, contraception,” the CEO says.
“I think it all came from personal experience and we all felt that it was an issue. Our chief medical officer, Dr Aaron Lazorwitz, is an OBGYN doctor and he experienced it in clinic, whereas myself and Paulina Cecula [her co-founder] experienced it as women. Paulina is also a medic and she was seeing that actually, doctors were having difficulties and the whole thing ended up being like ‘try this and come back if there’s a problem’.
“We thought that there’s a huge inefficiency [within the system] in this day and age. Women shouldn’t be having to trial and error to find if something is good for them,” Rueda adds. “So that drove us to start doing screening tests, making everything a lot more personal and helping the medical community to make the best decisions when it comes to contraception methods.”
She says that at the heart of this, education and communication are extremely important. “Women and young adults need to be educated around the topic of contraception better,” the CEO says.
“Women especially feel unable to verbalise how they feel, they can’t actually communicate it. So part of our solutions through the screening process, is to ask the right questions that help women understand their bodies and have a better conversation with their doctor.
“For that reason, I think personalised medicine is the future because actually, this one-size-fits-all approach isn’t working. When it comes to medication, you really do need to get that personalisation because the inside of us is so different and so unique.
“With technology becoming cheaper, we have the tools and the ability to make it more personalised and that essentially means taking into account medical history, preferences, maybe some biomarker information and just putting them together to be able to tailor the right treatment option.”
Experts like Rueda believe that very often huge amounts of data are being lost because of a lack of a data tracking system and that subsequently, makes the entire research process harder. “A doctor doesn’t tell you ‘Hey, try this contraception and tell me how you feel’ and actually write a report on it,” she explains. “That information is, therefore, not being captured. That’s dangerous because so much information is not being taken into account.”
But how could data tracking help the medical world? “A doctor is always going to use quantitative and qualitative data to make decisions, so symptom-tracking is one of the most powerful things that we can do as patients,” Rueda adds. “Data has so much power because it helps you essentially prove your point in an argument and is the fastest way to get information and to accelerate research.”
Walking into the clinic, as a woman, and feeling empowered is something that the CEO would like to see in the future and she also hopes that her company will support all women equally.
“The most important thing [for Dama Health] is to be able to be as accessible as possible and help women from different backgrounds. That impact is really important for us and also just working with the medical community and trying to implement our screening tests that could be easily accessed by anyone.”
The team will also be recruiting for beta testers and clinical in Q4 of 2022. If you are UK-based, you can sign-up here to be part of future clinical trials and research programmes.
For more info, visit damahealth.com.
Pregnancy
Wales becomes first UK nation to unite maternity care under a single digital record

System C has completed the national rollout of BadgerNet Maternity across all seven NHS Health Boards in Wales. This is the first time any UK nation has unified its maternity care under a single digital record and patient-facing app.
With approximately 26,000 babies born annually in Wales, BadgerNet connects maternity information across organisational boundaries in the country.
Expectant parents can access their records, maternity appointments and key updates digitally through a single app, wherever they receive care while clinicians have secure access to the right information at the point of care.
The national three-year agreement across all Heath Boards replaces a patchwork of separate local systems and eliminates the need for paper hand-held notes.
Anthony Tracey is director of digital at Hywel Dda University Health Board, the final of the Welsh Health Boards to go live with BadgerNet.
He said: “The rollout of BadgerNet across Wales is a vitally important step forward in modernising our maternity services and providing a consistent service across the country.
“By giving expectant parents direct access to their information and enabling clinicians to share data more effectively, we are strengthening safety, transparency and consistency in maternity care nationwide.”
For expectant parents, the single digital maternity record transforms how they engage with their care.
Instead of carrying paper notes and repeating information at every appointment, parents can access key details, appointments and updates digitally, supporting more informed conversations and shared decision-making.
The result is greater transparency, fewer administrative frustrations and a more joined-up experience throughout pregnancy and into the postnatal period, regardless of which health board they fall under.
For clinicians and Health Boards, the joined-up approach reduces duplication and streamlines handovers across teams and sites. Information is digitally captured once and made available securely wherever it is needed, helping to minimise errors, reduce time spent tracking down notes and support more efficient multidisciplinary working.
At a national level, linking maternity data across Wales creates a foundation for safer, more consistent care.
Aggregated, standardised information enables earlier identification of trends and variation, supports evidence-based policy decisions and enhances long-term service planning.
With a comprehensive view of maternity activity and outcomes across the country, Wales is now better positioned to raise standards for parents, babies and families.
Guy Lucchi, managing director of healthcare at System C, added: “Delivering a truly national approach across all seven Health Boards is a significant achievement for Wales.
“One shared system means information flows with the patient, not the organisation.
“That reduces duplication, supports earlier identification of risk and frees up valuable clinical time.
“Crucially, linking maternity data at a national level provides powerful insight to drive improvement. Health Boards can benchmark, plan services with greater confidence and ensure resources are targeted where they are needed most, while expectant parents benefit from clearer communication and a more connected experience of care.”
Pregnancy
Early birth safer in high blood pressure pregnancies – study
Pregnancy
App tracks heart risk after high-risk pregnancies

A recent study developed a new “digital companion” to support the prevention and follow-up of maternal cardiovascular risk in women with pregnancy complications.
Cardiovascular disease, or CVD, is the leading cause of premature death and illness in women, yet sex-specific causes remain understudied and women are underrepresented in research.
Pregnancy complications, including hypertensive disorders of pregnancy, or HDP, and gestational diabetes mellitus, or GDM, are strong predictors of future CVD, with pregnancy itself acting as a natural stress test.
Despite CVD accounting for 35 per cent of female deaths worldwide in 2019, systematic postpartum prevention remains limited in practice and incidence continues to rise.
Myocardial infarction, commonly known as heart attack, and stroke are the main fatal CVD events in women. Up to one-third of women develop hypertension within a decade after HDP, especially as maternal age rises.
Obstetric guidelines have historically lacked clarity on early CVD prevention after HDP and GDM, often relying on expert consensus rather than evidence.
Some cardiology guidelines now recommend personalised approaches, such as periodic hypertension and diabetes screening. Norwegian guidelines recommend cardiovascular risk evaluation at three months and one year postpartum, but adherence in practice is uncertain.
Effective risk reduction requires intervention before middle age. The immediate postpartum period following HDP or GDM is a critical window for early detection and intervention, offering an opportunity to engage women in cardiovascular health management, particularly as pregnancy can encourage long-term lifestyle awareness.
Electronic health, or eHealth, refers to the use of digital technologies and electronic communication tools to support healthcare services, medical information management and related health activities.
Systematic, eHealth-supported postpartum prevention can improve maternal health literacy and long-term cardiovascular outcomes.
However, there is a significant gap in targeted, eHealth-based postpartum interventions for cardiovascular risk management after HDP and GDM, despite strong patient demand and international calls for coordinated digital health strategies.
Home blood pressure monitoring shows promise, but broader digital support remains limited.
A cardiovascular postpartum follow-up programme was created as a mobile app based on Norwegian and international guidelines.
The MumCare app was developed through co-creation involving users, stakeholders and clinical experts. Five qualitative interviews and 10 user testing sessions informed improvements.
This study primarily analysed the iterative co-creation process used to develop the app, rather than evaluating clinical outcomes.
The MumCare project team in Oslo included an IT expert, obstetricians, a midwife, a GP, two sociologists and two cardiologists, all with relevant experience in eHealth and women’s health. A medical student with technological and medical expertise also helped turn ideas into app features for young women.
User representatives from two national patient associations contributed to information, recruitment, design and testing of the MumCare app.
Both associations provided user perspectives and took part in interviews and app testing. Additional users with HDP or GDM at Oslo University Hospital were also involved throughout the co-creation process.
The app’s digital infrastructure prioritises security and privacy, using encryption, de-identification and two-factor authentication.
User data is stored securely on the app and, for research purposes and with consent, on a dedicated University of Oslo server in line with GDPR and Norwegian regulations.
A linear Stage-Gate model structured the co-creation process, dividing it into phases with quality checkpoints reviewed in project meetings.
This approach balanced internal development with external user feedback, helping ensure the app is evidence-based, technically robust and user-centred.
The MumCare app guides postpartum women through tracking blood pressure, weight, physical activity and lab results, and provides personalised feedback to support self-management, mainly during the first postpartum year.
It also includes educational resources such as videos and guideline-based information to support understanding and engagement.
The app is also designed to support the transition from specialist pregnancy care to long-term follow-up with general practitioners.
It is described as a “digital companion” or health coach and does not replace clinical diagnosis or function as a medical device.
The co-creation process followed four phases focused on technical and procedural development.
In phase 1, input from expert organisations and user representatives established the app’s technical foundation.
It also reminds users of the one-year postpartum follow-up with their GP, a key time to assess risk factors and future care needs.
User organisation representatives gave feedback in phase 1, directly guiding content and feature development.
Phase 2 interviews confirmed that users want to monitor cardiovascular risk factors after HDP and GDM.
The analysis highlighted three themes: self-care strategies and uncertainties about hypertension, the need for accessible health information, and a more personalised approach to blood pressure monitoring in the app.
Concerns were also raised that frequent monitoring or app use could increase stress or create a sense of burden.
In phase 3, the app’s design and features were revised in response to feedback to improve usability and make sure they met users’ needs.
These changes led to a more intuitive and supportive interface for women during and after pregnancy.
Phase 4 involved building a prototype based on the updated designs, followed by further refinements after testing by the project team and users. Initial pilot testing with a small number of users suggested the app met its objectives and functioned as intended.
The MumCare app was co-created with input from experts, user organisations and patients over four phases.
Early expert and organisational contributions helped define the app’s goals, while ongoing feedback from patients helped ensure the design and content reflected users’ real needs.
This collaborative approach resulted in an app tailored to support women with pregnancy complications.
The MumCare app is currently being evaluated in a randomised controlled clinical trial that began in June 2024, with results needed to determine whether it improves long-term cardiovascular outcomes.

 Opinion4 weeks ago
Opinion4 weeks agoWhat Maternal Mental Health Month reveals about where postpartum support actually breaks down

 News3 weeks ago
News3 weeks agoNIH Grant terminations disproportionately impact minority scientists, research finds

 Menopause5 days ago
Menopause5 days agoPerimenopause misinformation ‘putting women at risk’

 Adolescent health3 weeks ago
Adolescent health3 weeks agoWUKA brings Period-Positive Pool Party to London Aquatics Centre to keep girls swimming through puberty

 Insight3 weeks ago
Insight3 weeks agoPCOS renamed after decade-long campaign to end ‘cyst’ misconception

 Events4 weeks ago
Events4 weeks agoWHIS 2026 unveils agenda and first speakers for the leading women’s health summit

 Menopause3 weeks ago
Menopause3 weeks agoCBT shows promise for menopause insomnia and hot flashes

 Insight4 weeks ago
Insight4 weeks agoOnline abuse and deepfakes ‘pushing women out of public life’





























Pingback: Pill problems: Why are women still struggling to access the right contraception, and how can healthtech help? - FemTech World