Mental health
Interview: The race to close the gap on late-stage breast cancer diagnoses

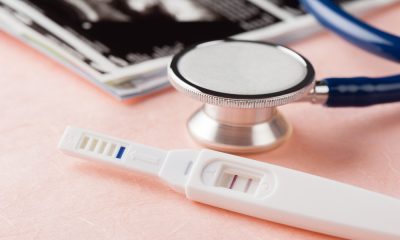
New research suggests that one in three eligible women in the US skip recommended mammograms – leading to late-stage breast cancer diagnosis, doubling treatment costs and increasing risk. Dr. Rani Aravamudhan, senior medical director at Nomi Health, speaks to Femtech World about addressing the problem, by helping employers and healthcare providers to reach women eligible for mammograms.
As part of its Trends in Spend series, Nomi Health has examined breast cancer screening and treatment data, finding that delayed detection negatively impacts patient outcomes and significantly increases financial burden.
Key findings from the report reveal that, while screening rates among women aged 40 to 74 have improved in recent years, over one-third continue to miss mammograms screenings at the recommended frequency, leaving significant gaps in preventive care.
Nomi highlights that unscreened women with advanced-stage breast cancer face treatment costs of up to US$120,485 which is US$44,029 more than screened patients at the same stage.
They are also more than twice as likely to be diagnosed with metastatic cancer.
Improving access and awareness
Currently, women over 40 are recommended to have a mammogram screening annually or bi-annually.
However, despite the year-over-year rate slowly trending upwards, still only around 63 per cent of eligible women are receiving their mammograms.
In order to improve screening uptake, Aravamudhan emphasises the importance of increasing awareness of mammograms.
“Despite the amount of data showing that mammograms are available at no out-of-pocket cost, not all women are aware of this – and I say that sympathetically- the healthcare system can be confusing,” says Aravamudhan.
“People wonder: what’s covered under my plan? I believe the system has become unnecessarily complex over the years, and that complexity discourages people from seeking care when they should.
“Certain services like annual physicals, mammograms, and colonoscopies must be made available to everyone at zero out-of-pocket cost.
“However, whether that’s true depends on someone’s insurance – often only if they go to an in-network facility. If they go out-of-network, they might still be charged. Understanding what’s in-network and what’s not can take real effort.”
Another barrier to mammogram uptake is access to these screenings, says Aravamudhan, highlighting that even in urban areas with ample facilities, getting an appointment isn’t always easy, with long wait times pushing back diagnoses.
“Even if financial access is fine, practical access is another issue. You need somewhere close by that can see you soon,” says Aravamudhan.
“In a rural or lower-income area, someone might need to travel 30 minutes or more just to reach a facility, they may have to take half a day off work for a 20-minute procedure.
“This is a very real, very practical problem. There are currently encouraging efforts though – some organisations, whether non-profits, hospital systems, or insurers have mobile units that go out to communities. These allow women to come to the unit, get their mammogram, and go.
“This is the kind of accessibility we need to expand.”
Aravamudhan suggests that these mobile units could also visit workplaces and retail stores to improve screening accessibility and reduce time needed off work for women.
“When we talk about access, it’s multi-layered,” says Aravamudhan.
“A relationship with a primary care provider (PCP) is also vital. Studies consistently show that when patients have a strong relationship with a PCP – someone who regularly checks in and encourages them to get screened – they are more likely to follow through.
“That trusted relationship leads to better compliance. And it’s not just mammograms – the same goes for Pap smears, colonoscopies, and so on.
“The provider doesn’t need to be forceful, just clear that this matters. It helps when they explain why it’s important and follow up. That relationship with a PCP matters a lot – not only for preventative screenings but for so many aspects of healthcare.”
Effective intervention for better outcomes
Awareness and access issues are contributing to delayed diagnosis, and Nomi’s analysis reveals that delayed diagnosis leads to an increase in the severity of treatment required.
Aravamudhan says employers, health plans, and healthcare providers all have a role to play in intervening more effectively to promote early detection.
“Employers are the ones providing health insurance for their employees and their dependents, so they have a significant stake in all of this,” says Aravamudhan.
“It’s crucial that we all – collectively – promote the value and benefits of preventive care early and often.
“It’s not just about getting a test or having a screening. It’s about investing in the health of our population. As individuals, we have a responsibility to do that for ourselves too. If I don’t invest in my own health, I risk having health issues that could impact my ability to work – and that, in turn, affects my family.
“Employers and health plans can do more during annual enrollment periods – not just talk about plan options, but also highlight the importance of preventive care with clear, relatable examples.
“They can share real stories – with permission – or public examples, such as someone well known who caught cancer early through screening and is now doing well. That kind of storytelling works and makes it real.
“Just like we reassure our children before a dentist visit, we need to normalise preventive care. It’s uncomfortable, but not painful – and it only takes 20 minutes. That kind of messaging – from colleagues, managers, health champions – can make a big difference.
“Reminders also help – as long as they’re targeted. Younger people may respond better to texts or emails, older people to phone calls. Tailor the channel to the audience.”
Another tool employers could utilise are incentives, says Aravamudhan, highlighting that many employers have healthcare rewards schemes
“Data shows that only a small percentage of people maximise those benefits,” says Aravamudhan.
“So there’s a lot of room for improvement – and a lot of opportunity to drive better engagement and health outcomes.”
Preventative care as a cost containment strategy
The Nomi analysis revealed that women who did not go for their mammograms who are diagnosed with advanced-stage breast cancer face treatment costs of up to $120,485, a total of $44,029 more than screened patients at the same stage.
The average cost per breast cancer episode was $25,765 for unscreened women, 18 per cent higher than for those who received their routine screenings.
In order to prevent these costs, Aravamudhan says that investment is needed in preventive care – whether employers, individuals or the wider system.
“I’m talking about continuous preventive care – a consistent, system-wide approach,” says Aravamudhan.
“It starts with disease prevention – such as vaccinations, for example. We absolutely should be promoting vaccines. We’ve already seen the consequences – falling vaccination rates in some areas like Texas have led to outbreaks of measles. Children are being hospitalised, some placed on ventilators, and tragically, some have died. That’s the real cost – not just financial, but lives lost.
“The next level of preventive care is screening. If someone is going to develop something like breast or cervical cancer, let’s catch it early.
“Early detection means a far better chance of survival and a much lower cost of treatment.
“Preventive care evolves into monitoring. We don’t just walk away after someone’s been treated for cancer – we continue to monitor them to make sure it doesn’t return, or to catch any new risks early. That’s still preventive care – just at a different stage.
“There is also chronic condition management. That might mean lifestyle changes, medication compliance, following a low-salt diet – whatever it takes. That kind of support system is key.
“And let’s not forget mental health. People often overlook preventive care in this space, but it absolutely exists. Building strong, consistent relationships with clinicians – whether through your GP, your insurer, or a nurse care manager – really matters.
“Those ongoing connections ensure preventive care stays front and centre. It helps reduce the long-term impact of conditions, and it lowers costs over time.
“All of this leads to healthier, happier families – and ultimately, far lower costs for employers. The alternative is simply more expensive – financially, socially, and emotionally.”
Menopause
More research needed to understand link between brain fog and menopause, expert says

Brain fog in menopause is common but still poorly understood, with researchers calling for more work to explain the link and how best to support women.
For a new perspective article published in The Lancet Obstetrics, Gynaecology, & Women’s Health, researchers based in the UK and Australia reviewed the evidence on menopause-related cognitive symptoms. They found that symptoms such as forgetfulness, reduced concentration and brain fog are common during the menopause transition, but are still poorly recognised and under-researched.
More than two-thirds of women report difficulties with memory or concentration over the menopause transition. Multiple factors may contribute to these cognitive symptoms, including hormonal changes, sleep disturbances and psychological and psychosocial stress. Yet, because cognitive symptoms are not widely discussed, they can cause considerable worry, with some fearing they are signs of dementia or undiagnosed neurodevelopmental conditions.
The review paper emphasises that overall cognitive performance for women experiencing menopause-related brain fog typically remains within expected ranges and, importantly, that cognitive symptoms are not linked to an increased risk of dementia.
Professor Aimee Spector of UCL Division of Psychology and Language Sciences, co-author on the paper, said: “Cognitive symptoms such as forgetfulness and ‘brain fog’ are incredibly common during menopause, yet they are often overlooked. Our findings highlight just how complex menopause-related cognitive symptoms are, and how much we still don’t know about what drives them. More targeted research is essential if we are to identify which biological, psychological or lifestyle factors contribute most, and what types of support or treatment are likely to be effective.”
The authors argue that clinicians can play a key role in understanding and validating women’s experiences by asking about the duration of cognitive symptoms, impacts on day-to-day functioning and any other medical or psychosocial factors that could be contributing to cognitive symptoms.
The review also discusses a range of approaches that may ease cognitive symptoms, such as improving sleep quality, engaging in regular aerobic exercise and eating a balanced diet. There is also little but promising research into the impact of psychological therapies targeting cognitive symptoms, with a recent meta-analysis of three cognitive behavioural therapy-based studies showing significant improvements in memory and concentration. The evidence is more mixed for the benefits of hormone therapy on cognitive symptoms during menopause.
The authors identify cognitive symptoms as a major area of unmet need in menopause research. They call for a unified definition of menopause-related cognitive changes and for prospective, longitudinal studies that can track women from pre- to post-menopause. Better understanding of the biological, psychological and social factors that contribute to cognitive symptoms will be crucial for developing effective treatments.
Lead researcher Dr Caroline Gurvich of Monash University said: “There’s a lot of pressure to use objective measures of cognitive decline, like a memory test, for example, in a clinical trial, but the key symptom of brain fog is a subjective experience. So having a definition that acknowledges the key cognitive symptom is critical.”
This is not without precedent – we already use subjective or self-report measures for depression, anxiety and other mental health conditions with great success.
Dr Gurvich said the proposed definition would also validate women’s individual experiences while empowering them through the reassurance that any objective decline in their cognitive ability is subtle.
She added: “This is a decrease in cognitive or learning efficiency, not functionality or capacity. For many women, the perception they are losing capacity is what drives them to stop work or lose the confidence to live fulfilling lives during and after menopause. I hear all the time from women who have gone through menopause that validation would have made a significant difference to their resilience and the approach they took to living with menopause.”
Co-author Professor Martha Hickey of the University of Melbourne and Royal Women’s Hospital said: “Our analysis of the best available research shows that many women experience some degree of cognitive symptoms, such as brain fog, during the menopause transition.”
“But there’s a lack of long-term data, which means that there’s a gap in our knowledge about how the brain fog symptom develops and changes from peri-menopause to after menopause ends. It’s a real gap in our understanding.”
Professor Spector added: “We increasingly see women, typically at the peak of their careers, losing confidence in the workplace, often translating to leaving work or reducing work hours. Having simple strategies to support and retain them at work is also a broader economic issue.”
Mental health
Inflammation linked to depression in women with diabetes, study finds

Inflammation may help flag depression in women with type 2 diabetes, new research reveals, but the link appears to vary by symptoms and by how depression is measured.
The findings suggest both the promise and the challenge of identifying biomarkers, measurable indicators in blood or other tests, for depression.
Women with type 2 diabetes are at higher risk of depression, which can accelerate diabetes complications, impair functioning and increase the risk of death. Research suggests inflammation may be a key link between the two conditions, as certain inflammatory biomarkers are frequently found in both.
Scientists have yet to identify an objective diagnostic biomarker for depression, such as something measured through blood work, a genetic test or a brain scan.
To diagnose and measure depression, mental health providers usually use questionnaires. Some add up the number of symptoms as a checklist, while others measure the severity of different symptoms.
Depression can also look very different from one person to the next, with symptoms spanning physical effects such as sleeping too much or too little, mood-related issues such as persistent sadness, and cognitive difficulties such as trouble concentrating.
Nicole Beaulieu Perez, assistant professor at NYU Rory Meyers College of Nursing and study author, said: “Depression is the most measured construct in all of science, but part of our problem is that we’re not defining depression the same, there may be different types, but we’re lumping them all together.
“The variability in depression symptoms complicates how we diagnose and treat it, particularly in the absence of validated biological markers.”
To better understand the connection between inflammation and different symptoms and measures of depression, researchers at NYU Rory Meyers College of Nursing studied 38 women with type 2 diabetes, many of whom were also living with HIV.
They analysed blood samples for 10 different inflammatory biomarkers, including CRP, IL-6, IL-4 and IL-8.
They also assessed participants for depression using PROMIS, an NIH-developed series of short questionnaires that includes measures of depression, anxiety, sleep and fatigue, as well as the CES-D, an older measure that adds up depression symptoms.
The researchers found that certain inflammatory biomarkers were linked to depression, but the associations varied depending on the measures and symptoms used.
Higher levels of depression and anxiety measured using PROMIS were associated with lower levels of IL-4.
They also found contradictory associations for CRP and IL-6. Both were positively correlated with depression when it was measured using CES-D and negatively correlated when it was measured using PROMIS.
Sleep disturbances measured using PROMIS were associated with IL-8.
Perez said: “It was interesting to see that, in some cases, the direction of these associations flipped entirely based on which measure of depression we were using.”
The findings, while preliminary because of the small number of people studied, suggest that the link between inflammatory biomarkers and depression may not be consistent across all measures or symptoms.
More research is needed to tease out the role of inflammation and whether subtypes of depression can be identified based on symptoms and objective biological markers.
Perez said: “We think there’s something going on with inflammation and depression, but if we look closely, we may find that’s true for some forms of depression but not others.”
She said she hoped that in future, pairing depression measures with biomarkers such as blood tests could provide more objectivity in diagnosing depression, which could help further destigmatise mental illness, as well as help clinicians catch it earlier and guide treatment.
Perez said: “Precision mental health has great potential.
“If we can identify a specific type of depression, for instance, one that appears to be driven by inflammation, this may inform which medications to try to target an underlying biological pathology, hopefully reducing the trial and error often needed to find an effective treatment for depression.
“By identifying specific inflammatory biomarkers linked to different dimensions of mental health, our findings suggest a path toward precision mental health that moves beyond one-size-fits-all approaches.”
Pregnancy
Miscarriage cradle to be rolled out across Scotland

 Entrepreneur2 weeks ago
Entrepreneur2 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Menopause4 weeks ago
Menopause4 weeks agoCalifornia plans US$3.4m menopause care overhaul

 Pregnancy3 weeks ago
Pregnancy3 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Menopause3 weeks ago
Menopause3 weeks agoWatchdog bans five ads for women’s heath claims

 Entrepreneur4 weeks ago
Entrepreneur4 weeks agoWHIS USA 2026 announces first ticket release for landmark Women’s Health Innovation Summit

 Menopause4 weeks ago
Menopause4 weeks agoMenopause has no lasting impact on cognition, research finds

 News2 weeks ago
News2 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Opinion3 weeks ago
Opinion3 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up