Wellness
Women have a far higher risk of dementia – and urgent action is needed

Recently published research has turned an overdue spotlight on the disproportionate burden of dementia borne by women. It is encouraging to see this research progressing, and inspiring to see it stimulating public awareness and discussion of a disparity that has too long been overlooked: women are twice as likely as men to develop Alzheimer’s disease.
By Andrea Pfeifer
We have been searching for new treatments for Alzheimer’s disease for decades and are now able to offer patients medicines that can slow the rate of memory loss. The research that led to the approval of these effective new medicines created a tremendous bank of knowledge about how Alzheimer’s causes damage to the brain – knowledge that enables us now, for the first time, to work on strategies to prevent damage before it happens.
As much as we have learned, however, we still do not understand why women are more prone to developing dementia and Alzheimer’s than men, nor do we know whether or how approaches to diagnosis, treatment and prevention should differ based on sex.
Researchers around the world are urgently studying questions about what causes these differences, and what they mean for treatment and prevention. In addition, new and exciting research is investigating sex-based differences in the effects of lifestyle and environmental factors that could lead to precision prevention approaches tailored for women and for men.
For this research to continue, its crucial to support public health strategies – and for us to continue to talk about dementia risk with the women in our lives to raise awareness of the ways we already have to preserve brain health.
Factors at play
Worldwide, about two-thirds of people living with Alzheimer’s are women. Women face a disproportionate burden in terms of care and lost economic productivity, and this is true across high-, middle- and lower-income countries.
Multiple reasons have been suggested to explain this difference. Among the hypotheses are higher life expectancy in women, because age is a risk factor for Alzheimer’s, and lower education in women, because limited education also is a risk factor. Geographical differences have been found, and we also know that one of the genetic factors that increases the risk of Alzheimer’s, a gene variant called APOE e4, has a stronger effect in women.
Women who carry APOE e4 are more likely than male carriers to accumulate toxic proteins in the brain, called amyloid plaques and tau tangles, which drive the loss of memory and cognition in Alzheimer’s. In addition, women who have amyloid and tau accumulation have faster disease progression rates compared with men.
Hormonal changes, particularly the decline in oestrogen during menopause, also may contribute to increased Alzheimer’s risk in women. But all women experience menopause, and not all women develop Alzheimer’s, so researchers are still working to understand how and why changes in hormones affect Alzheimer’s risk.
A study recently published in Science Advances by a team at Massachusetts General Hospital led by Dr. Gillian Coughlan investigated associations between hormone therapy and tau accumulation in menopausal women. The results further support a role for hormones in Alzheimer’s, and also highlighted a highly complex relationship between hormones and other factors such as age that need continued study.
Environmental and lifestyle factors also play a role in Alzheimer’s risk, and we are just beginning to study whether there are sex-based differences here as well.
All of these factors need more study, and understanding how they combine to affect risk for women as a group and for men and women as individuals will take time. Fortunately, there is a clear path forward.
Charting a way forward
The balance between women and men in clinical trials for Alzheimer’s treatments, which have historically underrepresented women, have improved in recent years. Yet detailed analyses of sex-specific differences in these studies are still lacking.
For example, trials of both the new Alzheimer’s medicines showed some difference in treatment results for women vs. men. However, neither trial was designed to draw conclusions about how important or meaningful those differences are, or to understand whether such differences could be related to other factors such as hormone profiles, education, and so on.
Going forward, we need to ensure that the participation of women and men in clinical trials reflects the prevalence of Alzheimer’s in both sexes. There is a need for sex-based data collection and analysis across all stages of research, from basic biology research to clinical trials.
One way to ensure this is to make the integration of sex and gender in research plans a requirement for funding or publishing. Another is to enhance diversity in teams in research, policy, and healthcare practice.
We also need to redouble our efforts to reduce dementia risk globally, and to increase awareness of the tools that we already know can make a difference.
My goal, as the CEO of a biotech working in Alzheimer’s disease and the co-founder and Chair of the Global BHP Braintrust, is to develop and promote effective strategies to reduce the overall risk of dementia using a Precision Prevention approach that includes active immunotherapy and lifestyle changes.
Active immunotherapy is a type of medicine that stimulates the immune system to clear or prevent the accumulation of pathological proteins like amyloid or tau. These medicines are still in development but could be available in as little as five years.
Lifestyle interventions enable everyone to target modifiable risk factors such as diet, exercise, cognitive and social stimulation, and vascular health.
It is estimated that at least 40 per cent of cases worldwide can be linked to modifiable facets of lifestyle including cardiovascular, metabolic and environmental factors. A landmark study called the Finnish Geriatric Intervention Study to Prevent Cognitive Impairment and Disability (FINGER) showed that a multi-faceted lifestyle intervention program could improve brain health and prevent cognitive decline by about 30 per cent.
The intervention combined healthy food, physical activity, mental stimulation, social activities, and cardiovascular risk monitoring.
The benefit of the intervention on cognitive outcomes did not differ significantly between men and women. Sex-specific differences in certain cognitive domains, as well as in the adoption of lifestyle changes, point to the opportunity to further improve the impact of the intervention.
The Global BHP BrainTrust is now collaborating on FINGERS Plus for Women, a research initiative to explore the potential for gender-specific interventions to further reduce the risk of dementia.
A better future
Used together, both active immunotherapy and lifestyle interventions could enable a more personalized risk reduction strategy based on an individual’s sex, genetic risk, biomarkers, and lifestyle factors.
Many of us have family or friends who suffer from dementia. We know that it is a global scourge that silently ravages millions of lives.
Together with other researchers, companies, and policymakers, we have the capacity to close the gap between women and men, addressing this pressing public health concern for all.
Prof. Andrea Pfeifer is co-Founder and CEO of AC Immune, a Swiss biopharmaceutical company pioneering precision prevention for neurodegenerative diseases. She has led the company since founding in 2003 and through an IPO and multiple partnerships with leading pharmaceutical companies. She was previously Head of Nestlé Research Centre, where she played a major role in connecting science and business.
Prof. Pfeifer is a key member of the CEOi initiative on Alzheimer’s Disease and the Davos Alzheimer’s Collaborative (DAC), a Founding Chair of the Global BHP Braintrust, and in 2021 was awarded the first SEF.WomenAward for CEO of the Year by the Swiss Economic Forum. She holds a Ph.D. in Toxicology (Cancer Research) from the University of Würzburg, Germany and is an Honorary Professor at the Ecole Polytechnique Fédérale de Lausanne (EPFL).
Adolescent health
Newly-launched Female Health Hub will support grassroots football players

A new Female Health Hub launched by the English FA will support women and girls in grassroots football in England with trusted advice on health issues affecting play.
The hub brings together expert-backed guidance, practical tools and player insights in one place, giving women and girls practical advice and reassurance on female health in football.
It has four core aims: to help women and girls better understand their bodies and how female health affects performance and participation, to educate players on key health topics and when to seek further advice or support, to provide practical strategies to help navigate common female health challenges, and to help break down taboos and normalise conversations around female health in football.
Users of the hub will also be able to hear directly from members of the England women’s national team, who share their own experiences of navigating female health matters while playing at the highest level of the game.
“Our ambition is to create a game where women and girls can thrive,” said Sue Day, the FA’s director of women’s football.
“To achieve that, it’s essential that players feel supported in environments that understand and respond to their female health needs.
“We’ve heard directly from grassroots players that they want better information and support around female health, but that they often don’t know where to find it.
“The launch of the Female Health Hub marks an important step in changing the landscape.
“We want every player to feel confident in her own skin and supported without judgment, so she can feel empowered by her body, rather than held back by it.”
The platform was launched following research conducted by the FA that highlighted the need for better education and support around female health in football.
According to the FA, 88 per cent of adult players surveyed said their menstrual cycle has an impact on their ability to train or play, but 86 per cent reported they had never received education about the menstrual cycle in relation to football performance and training.
The research also found 64 per cent of women experience issues related to sports bras or breast health while playing football, despite sports bras being considered one of the most important pieces of playing kit.
Players also expressed strong interest in learning more about injury prevention, at 87 per cent, nutrition, at 84 per cent, and mental health, at 77 per cent, in relation to female health.
The first phase of the Female Health Hub focuses on three of the most requested topics: menstrual health, breast health and injury resilience, with further content to follow, including nutrition and pelvic health guidance.
Menopause
New Women’s Employment Ambassador role targets workplace health
Pregnancy
Physicians neglecting preventive care for women with diabetes, study finds
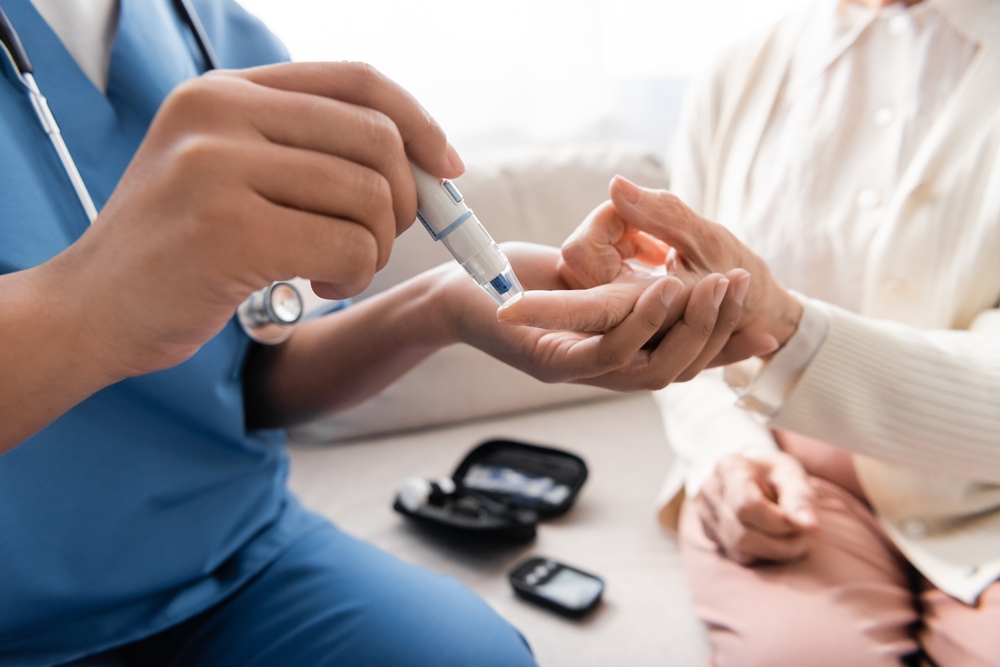
Women with diabetes are less likely to get preventive care than those without the condition, a UCLA-led study suggests.
The findings are based on an analysis of more than 40 studies from several countries.
They highlight how physicians largely overlook the importance of these routine services for women who have diabetes mellitus, or DM, putting them at risk of preventable medical conditions such as pregnancy complications.
Lauren Wisk is associate professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA and senior author on the study.
She said: “These findings are important because they identify that women with diabetes are not receiving recommended well-woman care, which is essential to support both managing their diabetes and their overall health.
“Providers need to be aware that they should not forget to provide these essential services for women with diabetes.”
The researchers sifted through thousands of studies, focusing on the concepts of women, diabetes and women’s health services, and settled on 44 that addressed treatment services for women aged 15 to 49 with type 1 or type 2 diabetes, excluding those with diabetes insipidus or gestational diabetes.
They looked at four preventive health service categories: contraceptive counselling and use, breast and cervical cancer screening, pre-conception counselling, and screening for sexually transmitted infections.
One study found that 48 per cent of women with diabetes received contraceptive services compared with 62 per cent of women without the disease.
Nine papers showed cervical cancer screening rates ranging from 38 to 79 per cent for women with diabetes compared with 46 to 86 per cent for those without diabetes.
Four studies found that breast cancer screening rates for women with diabetes ranged between 38 and 69 per cent compared with 54 and 82 per cent for those without diabetes.
Fourteen studies found pre-conception counselling rates of just over 1 per cent compared with 46 per cent for women with diabetes who are planning to get pregnant.
The researchers did not identify any studies on screening for sexually transmitted infections, which they said represents “a substantial gap in the literature.”
The researchers wrote: “One of the more striking findings of this review is the importance of robust coordinated care teams in ensuring access to appropriate services for women with DM.
“Several of the identified studies provide support that a co-management model, or the concept of involving endocrinology, primary care, and other specialty care providers in the care of individuals with DM, as recommended by the American Diabetes Association, is associated with greater receipt of services.”
Within the time constraints of an office visit, primary care physicians are expected to address preventative health needs as well as chronic disease management, said Dr Lisa Kransdorf, an associate clinical professor of medicine at the Geffen School and a study co-author.
She said chronic disease management will often take priority.
“In cases where the patient has other providers such as specialists and clinical pharmacists actively involved in their chronic disease management, there is opportunity for primary care physicians to attend to preventative care gaps,” the researcher added:
There are some limitations to the findings.
The search yielded only 44 studies, many of which relied on patient recall, which can be unreliable, highlighting the need for further research.
In addition, most of the studies analysed had small sample sizes or were conducted at a single site, limiting how applicable the findings might be in other settings.

 Entrepreneur2 weeks ago
Entrepreneur2 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Menopause4 weeks ago
Menopause4 weeks agoCalifornia plans US$3.4m menopause care overhaul

 Pregnancy3 weeks ago
Pregnancy3 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Menopause3 weeks ago
Menopause3 weeks agoWatchdog bans five ads for women’s heath claims

 Entrepreneur4 weeks ago
Entrepreneur4 weeks agoWHIS USA 2026 announces first ticket release for landmark Women’s Health Innovation Summit

 Menopause4 weeks ago
Menopause4 weeks agoMenopause has no lasting impact on cognition, research finds

 News2 weeks ago
News2 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Opinion3 weeks ago
Opinion3 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up




























