News
Scientists develop breakthrough approach to detecting endometriosis in menstrual blood
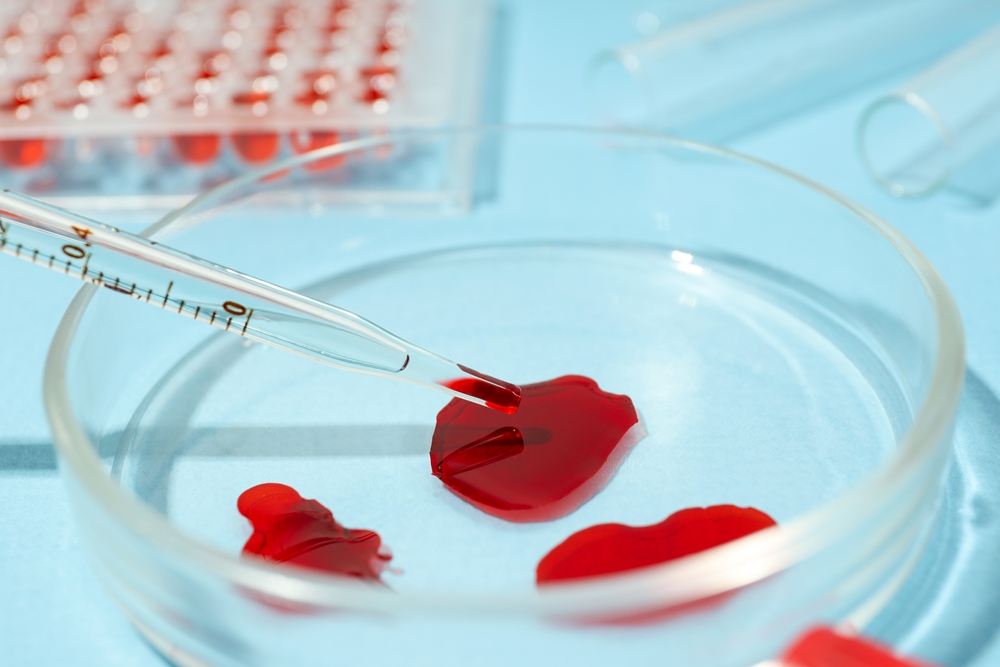
Scientists have developed a powerful new approach to detecting endometriosis which could transform how the disease is researched, diagnosed and treated.
In a world-first clinical study, scientists tested a pioneering diagnostic process which involves directly isolating menstrual blood-derived stem cells (MenSCs) from menstrual blood samples for analysis, rather than analysing cultured cells.
Scientists believe MenSCs are the cells that drive lesion formation in endometriosis.
Culturing the cells alters their make-up; whereas freshly isolating the cells without culturing preserves their molecular integrity, enabling a deeper and more direct view into how endometriosis behaves than ever before.
Dr Francisco Carmona is former president of the International Society of Endometriosis and Uterine Disorders, head of the Endometriosis and Uterine Transplant Unit at Hospital Clínic Barcelona, and co-author of this study.
The researcher said: “This study marks a significant leap forward in our mission to understand the biology of endometriosis.
“It has far-reaching implications: the methods tested could power the development of non-invasive patient stratification and diagnosis, better treatments and personalised care pathways, transforming the lived experience of patients with endometriosis and how we approach their care.”
In this landmark study, scientists were the first to analyse freshly isolated MenSCs using a process called DNA methylation profiling, which is already widely used to diagnose cancer.
They achieved an accuracy rate of 81 per cent and were clearly able to distinguish participants with endometriosis from those without.
The approach means scientists can use readily available menstrual blood samples to accurately diagnose and categorise endometriosis: a significantly less invasive process for patients than the current diagnostic gold standard, which involves a surgical procedure called a laparoscopy.
It also enables scientists to uncover critical information about the disease that can’t currently be provided by diagnostic imaging or biopsies.
Scientists hope the new technology will enable clinicians to detect endometriosis far earlier and without surgical intervention, reducing endometriosis diagnosis times from an average 7-10 years to just a few weeks.
The team also hopes to lay the foundation for the development of targeted therapies to treat different types of endometriosis.
Their approach could enable clinicians to stratify patients based on how the disease is behaving, and give patients access to targeted treatments before the condition has advanced.
The study was carried out by researchers at Hospital Universitario Insular de Gran Canaria and Hospital Clínic Barcelona – a leading centre in endometriosis care and research.
It was led by endogene.bio: a Paris-based precision medicine organisation on a mission to turn cutting-edge science into clinical tools that can close the female health gap. The endogene.bio team comprises world-leading experts in epigenetics, gynaecology, immunology and computational biology, many of whom also suffer from endometriosis.
Dr María Teresa Pérez Zaballos, co-founder and CEO at endogene.bio, said: “We wanted to design something that we as patients, but also as researchers, wished had existed.
“By accessing the molecular signals in menstrual blood, we’re unlocking information about endometriosis activity that was previously only available through surgery.
“Our approach shows DNA methylation profiling is a reliable, non-invasive way to diagnose endometriosis.
“Our findings also support the use of menstrual blood as a stable diagnostic sample.
“Many members of our team are endometriosis patients themselves, myself included. Our firsthand understanding of the diagnostic delays, clinical blind spots, and emotional toll of endometriosis shapes every decision we make, from sample collection design to clinical priorities.
“This is a company built by scientists who understand the molecular complexity of the disease and by patients who know exactly where medicine has fallen short.”
Mental health
Timing is everything: What AI need to learn about HRT and brain health

By Morgan Rose, CNM, WHNP-BC, and Dr Kudesia, triple board-certified in Reproductive Endocrinology & Infertility (REI), Obstetrics & Gynecology, and Lifestyle Medicine
The timing of when women start hormone replacement therapy (HRT) may matter more than we ever understood.
The “critical window” for starting HRT isn’t just relevant to brain health; timing has also been shown to shape cardiovascular outcomes.
Early analyses of the landmark WHI trial missed this nuance, including women long past menopause and obscuring benefits seen in those who begin therapy sooner.
Recent research presented at the American Neurological Association Annual Meeting found that women who began HRT within five years of menopause had a 32 per cent lower risk of developing Alzheimer’s disease.
Yet those who started HRT more than five years after menopause showed higher levels of tau proteins, a hallmark of Alzheimer’s, in their brains.
This “critical window” concept challenges the one-size-fits-all model of menopause care. It suggests that when we start HRT, it can be just as important as whether we start it.
Researchers at Mass General Brigham found similar patterns: women who began HRT near the onset of menopause did not show increased Alzheimer’s risk, while those who experienced early menopause with longer lifetime estrogen deprivation faced a higher risk overall.
Why Timing Matters
Women face roughly a 1 in 5 lifetime risk of Alzheimer’s disease, compared to 1 in 10 for men of the same age. The sharp drop in estrogen during menopause may help explain that gap.
Estrogen supports energy production, blood flow, and inflammation control in the brain functions that wane as levels decline.
The data suggest that initiating HRT earlier (around perimenopause or early menopause) may preserve some of these neuroprotective effects, while starting too late could heighten risk once neurodegenerative changes have already begun.
One meta-analysis showed that HRT begun soon after menopause reduced Alzheimer’s risk by over 40 per cent compared to non-users, while starting after age 60 doubled the risk.
These findings don’t make HRT a blanket prescription; they make it a precision intervention.
The Clinical Nuances AI Must Understand
If AI is going to support menopause care safely and intelligently, it needs to understand the reasons behind the actions.
1. Timing Is a Risk Modifier
“Time since menopause” is not just a demographic; it’s a clinical determinant.
AI systems must understand that the same therapy can carry opposite implications depending on when it’s initiated.
2. HRT Is Not Monolithic
There are multiple formulations, routes, and combinations.
For women who still have a uterus, adding progesterone helps protect the uterine lining and lowers the risk of endometrial cancer that can occur with estrogen-only therapy.
Topical estrogen, which has much lower absorption into the bloodstream, may be appropriate for perimenopausal women who are still having periods or postmenopausal women with a uterus who need targeted relief of vaginal or urinary symptoms.
For example:
- Estrogen-alone therapy can raise the risk of endometrial cancer and is typically not recommended for women with a uterus.
- Topical estrogen, with much lower systemic absorption, may be appropriate for perimenopausal women still having periods.
These distinctions must be explicitly encoded into AI frameworks to avoid oversimplified or unsafe recommendations.
3. Safety Requires Scope and Referral
Complex topics like HRT timing and neuroprotection should always prompt an automatic follow-up:
“Please consult a menopause specialist or clinician (such as one credentialed through the North American Menopause Society) to discuss the risks, benefits, and best options for you.”
AI logic must mirror how clinicians practice by inviting deeper discussion, not replacing it.
From Symptoms to Systems Thinking
We need to move beyond viewing menopause as a set of symptoms to manage, and instead see it as a neurological and metabolic inflection point in women’s lives.
That means:
- Bringing conversations about HRT earlier, during perimenopause, when neuroprotective benefits may still be possible.
- Designing AI systems that recognise context and chronology, not just keywords.
- Making personalised, evidence-based menopause guidance accessible to every woman by cutting through misinformation and connecting her to trusted care.
The Bigger Picture
For too long, women’s midlife health has been under-researched and under-resourced. The result is a data gap, which can quickly become a bias when encoded into AI.
If we want women’s health AI to truly care, it must be trained on data that understands the complexity of hormonal transitions, not just the vocabulary of them.
Because the difference between “now” and “five years from now” can determine whether a woman ages with clarity or confusion.
AI should know that.
And soon, it will.
Dr Kudesia is nationally recognised for her expertise in fertility awareness, lifestyle, and culinary approaches to reproductive health, and her advocacy for reproductive rights.
Hormonal health
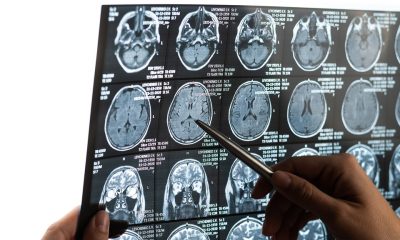
Women better protected against early Parkinson’s neurodegeneration, study finds
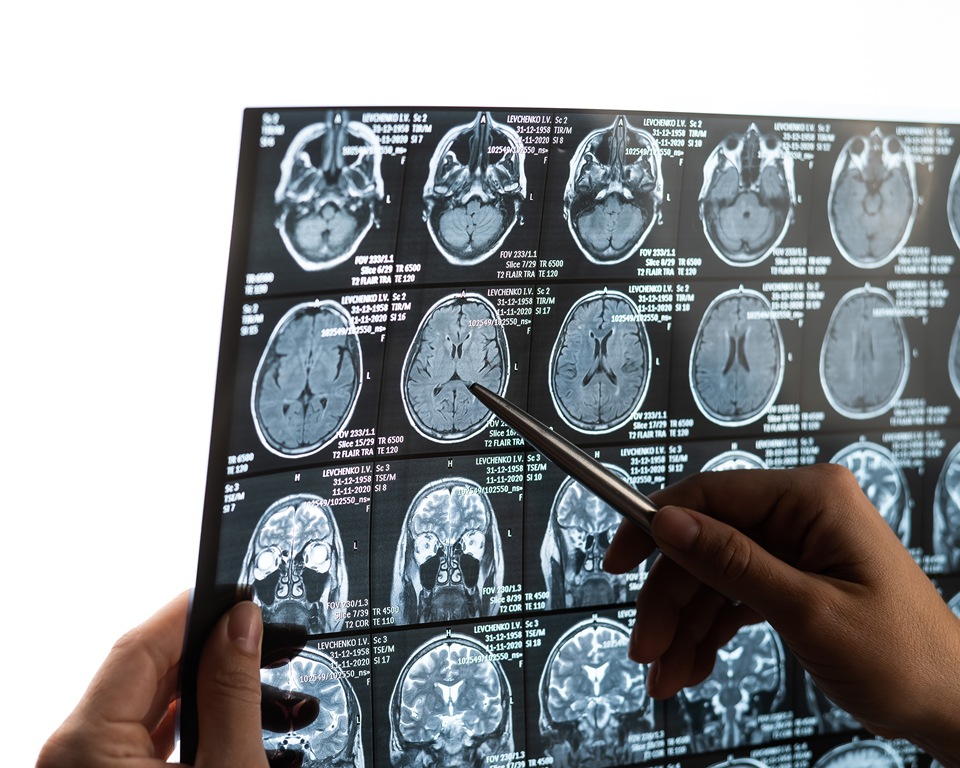
Women with an early precursor to Parkinson’s disease show much less brain shrinkage than men, despite similar disease severity, new research shows.
The discovery could help scientists explore how hormones might one day be used to treat the neurodegenerative condition.
The findings are based on data from nearly 700 participants across nine international research centres.
The study focused on isolated REM sleep behaviour disorder — a condition in which people physically act out their dreams.
It is considered the most reliable early warning sign of diseases caused by toxic protein build-up in the brain.
More than 70 per cent of those affected later develop Parkinson’s disease, Lewy body dementia or multiple system atrophy, which affects several body systems.
Researchers from Université de Montréal analysed 888 brain scans from centres in Canada, the Czech Republic, the UK, France, Australia, Denmark and Italy.
After quality checks, 687 participants were included: 343 patients with the sleep disorder and 344 healthy controls.
The results revealed clear sex-based differences.
While 37 per cent of the cortical areas — the brain’s outer layer responsible for higher functions — showed thinning in men, only one per cent of regions were affected in women.
This difference remained even though participants were of similar age (around 67) and had comparable clinical profiles.
Marie Filiatrault is first author of the study and a doctoral student at Université de Montréal.
The researcher said: “Men show much more extensive and severe cortical thinning — the outer layer of the brain that controls our higher functions — than women, particularly in areas linked to movement, sensation, vision and spatial orientation.”
To understand the protective effect, researchers compared brain images with gene activity in different regions, measured in healthy brains after death.
They found that the less-affected areas in women showed higher expression of genes related to oestrogen function, particularly ESRRG and ESRRA, which produce oestrogen-related hormone receptors.
The ESRRG gene was especially notable, showing greater activity in brain tissue than elsewhere in the body.
These receptors play key roles in mitochondrial function — the cell’s energy production system — and in the survival of dopamine-producing neurons, the cells that die in Parkinson’s disease.
Shady Rahayel is professor at Université de Montréal’s Faculty of Medicine and lead author of the study.
Rahayel said: “This sleep disorder offers a unique window of opportunity to study the mechanisms of neurodegeneration before major motor or cognitive symptoms appear.
“Our results suggest that certain brain areas in women with isolated REM sleep behaviour disorder are better protected than those in men, likely through the action of oestrogens.”
The team chose to study this precursor condition because it allows observation of brain protection mechanisms before major motor symptoms develop.
Although only 25 to 40 per cent of people with Parkinson’s experience REM sleep behaviour disorder, studying this early stage gives insight into how the brain resists damage when it is still limited.
Previous studies have shown that women with established Parkinson’s disease tend to experience slower progression than men, pointing to similar protective effects.
The findings could shape future research and treatment development.
The authors recommend separating men and women in clinical trials, which could improve statistical accuracy and reduce the number of participants required.
The biological mechanisms identified — particularly those linked to the ESRRG gene — could also become potential therapeutic targets.
Early laboratory research suggests that increasing ESRRG activity may protect dopamine-producing neurons from the toxic effects of alpha-synuclein, a protein that builds up abnormally in the brains of people with Parkinson’s.
“This study brings us closer to precision medicine, where treatments could be tailored not only to the disease but also to individual biological characteristics, including sex,” said Rahayel.
News
Dozens of women report suffering painful burns after using Always sanitary towels

Dozens of women have claimed online that Always sanitary towels caused painful burns, prompting a response from the Procter & Gamble-owned brand.
Several TikTok users have posted videos describing reactions to the company’s products in recent days.
The clips, which have gained thousands of views, include complaints of itching, rashes and what users describe as chemical burns — skin damage caused by contact with irritating substances.
In one video viewed 45,000 times, user @ratqueen910 said the pads gave her “the worst chemical burns ever” in her groin area, where underwear meets the leg.
“When I looked at the burn with the flash on it really looked like my skin was gooey! I was scared af,” she told commenters.
She said she first thought the pain was chafing or an allergic reaction to spandex in her underwear, before seeing other women online describe the same symptoms.
“I realised that so many people have had problems the last few months with these pads,” she said.
“It’s not like, ‘oh, I switched over to Always pads’ — no, I’ve used them since I was in like sixth grade.
“So they must have changed the formula, messed something up, put some extra chemicals in that sh**t because it messed me up. I had chemical burns. I had issues and I didn’t know what it was.”
She said a doctor suggested another cause for the irritation, but she believes the pads were to blame, noting she had never been sensitive to scents or suffered urinary or yeast infections before.
Her post drew hundreds of comments, with many women saying they too had reactions to Always’ Flexfoam pads.
One wrote: “The whole area that the pad touched gave me a chemical burn after only a few hours. It was the Flexfoam.”
The original poster replied: “Mine was Flexfoam as well.”
While users did not specify exact product types, Always sells both day and night versions of its Infinity Pads with Flexfoam, which appear to be those mentioned.
Another commenter said: “Just a few days ago I was on my period using Always pads and I was f**king itching and it was burning. I never itch or have pain down there. I took the pad off so quick.”
A third wrote: “I switched to Honey Pot and had been fine. When my coworker gave me an Always pad, I was hesitant but used it — and got a chemical burn.”
Others described repeated irritation.
One said: “I use another brand for the first half of my period, then Always for the last two days, and I’ve had this burn for three months in a row. Stopped using them last month and no issue.”
Some also reported rashes or itching. One wrote: “In real time I am itching and getting a rash. I wore an Always pad earlier today.”
An Always spokesperson told the Daily Mail: “Our pads are used safely by millions of women every day around the world.
“Their safety is our top priority, and we carefully evaluate every component of our Always products to minimise the chances of skin irritation or allergic reactions.”

 Menopause2 weeks ago
Menopause2 weeks agoFDA plans to revise black box warning on menopause hormone therapies

 News2 weeks ago
News2 weeks agoAI-powered women’s health companion Nexus launches in UK

 Fertility2 weeks ago
Fertility2 weeks agoScientists turn human skin cells into eggs in IVF breakthrough

 Wellness6 days ago
Wellness6 days agoWomen’s health innovations recognised in TIME’s Best Inventions 2025

 News2 weeks ago
News2 weeks agoDaily pill could delay menopause ‘by years,’ study finds

 News2 weeks ago
News2 weeks agoAncient herb to modern must-have: Why ashwagandha is capturing UK women’s attention

 Menopause3 weeks ago
Menopause3 weeks agoNew report exposes perimenopause as biggest blind spot in women’s health

 News1 week ago
News1 week agoMenstrual cycle affects women’s reaction time, study finds