Wellness
AI outperforms breast density for breast cancer risk

An artificial intelligence model predicts five-year breast cancer risk more accurately than traditional breast density assessment, new research shows.
The image-only AI model, called Clairity Breast, showed that women in its high-risk group had more than a fourfold higher cancer incidence than those in the average-risk group (5.9 per cent vs 1.3 per cent).
Breast density, which refers to the amount of fibrous and glandular tissue compared to fatty tissue in the breast, has traditionally been used as one indicator of cancer risk. Dense breast tissue can both mask tumours and slightly increase cancer risk.
Researchers from Harvard Medical School and University Hospital RWTH Aachen in Germany tested the FDA-authorised AI model on 245,232 screening mammograms from US and European sites taken between 2011 and 2017.
The AI was trained on 421,499 mammograms from 27 facilities across Europe, South America and the US, learning to identify subtle tissue patterns that predict cancer development within five years. It uses a deep convolutional neural network (a pattern-recognition algorithm) to generate risk probabilities.
Traditional density assessment showed minimal difference in outcomes: 3.2 per cent for dense versus 2.7 per cent for non-dense breasts.
“Over two million women are diagnosed with breast cancer annually, and for most, it comes as a complete shock,” said Dr Constance D. Lehman, professor of radiology at Harvard Medical School. “Only 5 to 10 per cent of breast cancer cases are considered hereditary, and breast density alone is a very weak predictor of risk.”
The AI categorised risk using National Comprehensive Cancer Network thresholds: average (less than 1.7 per cent), intermediate (1.7-3.0 per cent) and high (greater than 3.0 per cent) five-year risk.
“The model is able to detect changes in the breast tissue that the human eye can’t see,” Dr Lehman explained. “This is a job that radiologists just can’t perform. It’s a separate task from detection and diagnosis, and it will open a whole new field of medicine, leveraging the power of AI and untapped information in the image.”
The findings have particular significance for younger women. While the American Cancer Society recommends optional annual screening from age 40 for average-risk women, those under 40 represent the fastest-growing group diagnosed with breast cancer and advanced disease.
“An AI image-based risk score can help us identify high-risk women more accurately than traditional methods and determine who may need screening at an earlier age,” Dr Lehman said. “We already screen some women in their 30s when they are clearly at high risk based on family history or genetics. In the future, a baseline mammogram at 30 could allow women with a high image-based risk score to join that earlier, more effective screening pathway.”
Dr Christiane Kuhl, director of the Department of Diagnostic and Interventional Radiology at University Hospital RWTH Aachen, who presented the findings, emphasised the clinical implications.
“The results of this large-scale analysis demonstrate that AI risk models provide far stronger and more precise risk stratification for five-year cancer prediction than breast density alone,” she said. “Our findings support the use of image-only AI as a complement to traditional markers supporting a more personalised approach to screening.”
Currently, 32 US states have breast density legislation requiring healthcare providers to inform women of their density status after screening mammograms. The researchers suggest this information could be enhanced with AI risk scores.
“We’d like to see women given information on their breast density and their AI image-based risk score,” Dr Lehman said. “We can do better than just looking at a mammogram and saying, ‘It is dense or not dense’ to inform women of their risk.”
The technology represents what its developers describe as a shift in breast cancer screening from population-based to personalised risk assessment, potentially enabling earlier intervention for high-risk women while reducing unnecessary procedures for those at lower risk.
Adolescent health
Newly-launched Female Health Hub will support grassroots football players

A new Female Health Hub launched by the English FA will support women and girls in grassroots football in England with trusted advice on health issues affecting play.
The hub brings together expert-backed guidance, practical tools and player insights in one place, giving women and girls practical advice and reassurance on female health in football.
It has four core aims: to help women and girls better understand their bodies and how female health affects performance and participation, to educate players on key health topics and when to seek further advice or support, to provide practical strategies to help navigate common female health challenges, and to help break down taboos and normalise conversations around female health in football.
Users of the hub will also be able to hear directly from members of the England women’s national team, who share their own experiences of navigating female health matters while playing at the highest level of the game.
“Our ambition is to create a game where women and girls can thrive,” said Sue Day, the FA’s director of women’s football.
“To achieve that, it’s essential that players feel supported in environments that understand and respond to their female health needs.
“We’ve heard directly from grassroots players that they want better information and support around female health, but that they often don’t know where to find it.
“The launch of the Female Health Hub marks an important step in changing the landscape.
“We want every player to feel confident in her own skin and supported without judgment, so she can feel empowered by her body, rather than held back by it.”
The platform was launched following research conducted by the FA that highlighted the need for better education and support around female health in football.
According to the FA, 88 per cent of adult players surveyed said their menstrual cycle has an impact on their ability to train or play, but 86 per cent reported they had never received education about the menstrual cycle in relation to football performance and training.
The research also found 64 per cent of women experience issues related to sports bras or breast health while playing football, despite sports bras being considered one of the most important pieces of playing kit.
Players also expressed strong interest in learning more about injury prevention, at 87 per cent, nutrition, at 84 per cent, and mental health, at 77 per cent, in relation to female health.
The first phase of the Female Health Hub focuses on three of the most requested topics: menstrual health, breast health and injury resilience, with further content to follow, including nutrition and pelvic health guidance.
Menopause
New Women’s Employment Ambassador role targets workplace health
Wellness
Physicians neglecting preventive care for women with diabetes, study finds
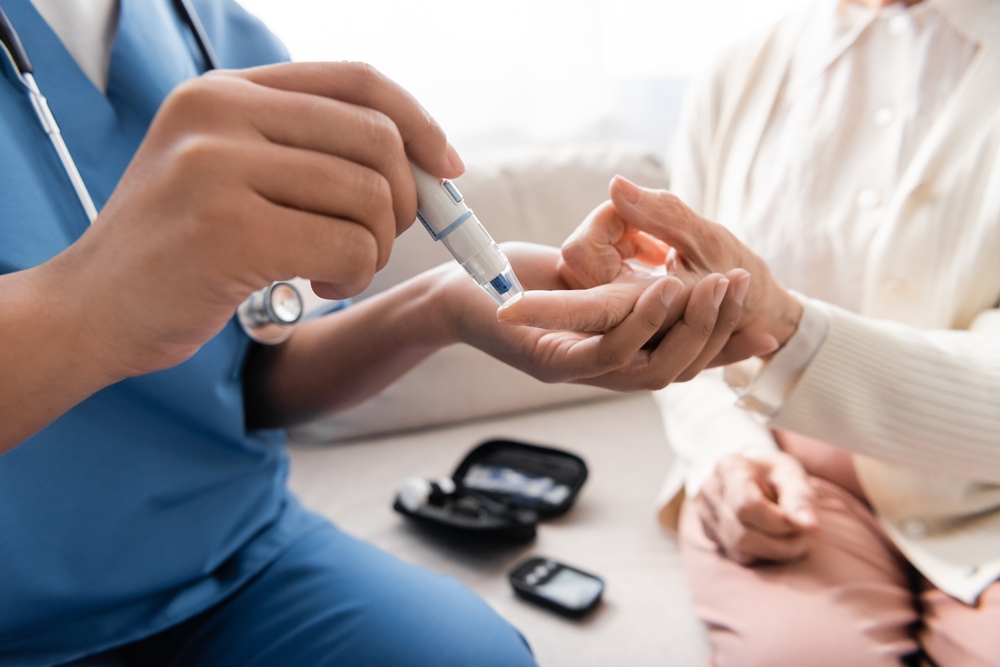
Women with diabetes are less likely to get preventive care than those without the condition, a UCLA-led study suggests.
The findings are based on an analysis of more than 40 studies from several countries.
They highlight how physicians largely overlook the importance of these routine services for women who have diabetes mellitus, or DM, putting them at risk of preventable medical conditions such as pregnancy complications.
Lauren Wisk is associate professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA and senior author on the study.
She said: “These findings are important because they identify that women with diabetes are not receiving recommended well-woman care, which is essential to support both managing their diabetes and their overall health.
“Providers need to be aware that they should not forget to provide these essential services for women with diabetes.”
The researchers sifted through thousands of studies, focusing on the concepts of women, diabetes and women’s health services, and settled on 44 that addressed treatment services for women aged 15 to 49 with type 1 or type 2 diabetes, excluding those with diabetes insipidus or gestational diabetes.
They looked at four preventive health service categories: contraceptive counselling and use, breast and cervical cancer screening, pre-conception counselling, and screening for sexually transmitted infections.
One study found that 48 per cent of women with diabetes received contraceptive services compared with 62 per cent of women without the disease.
Nine papers showed cervical cancer screening rates ranging from 38 to 79 per cent for women with diabetes compared with 46 to 86 per cent for those without diabetes.
Four studies found that breast cancer screening rates for women with diabetes ranged between 38 and 69 per cent compared with 54 and 82 per cent for those without diabetes.
Fourteen studies found pre-conception counselling rates of just over 1 per cent compared with 46 per cent for women with diabetes who are planning to get pregnant.
The researchers did not identify any studies on screening for sexually transmitted infections, which they said represents “a substantial gap in the literature.”
The researchers wrote: “One of the more striking findings of this review is the importance of robust coordinated care teams in ensuring access to appropriate services for women with DM.
“Several of the identified studies provide support that a co-management model, or the concept of involving endocrinology, primary care, and other specialty care providers in the care of individuals with DM, as recommended by the American Diabetes Association, is associated with greater receipt of services.”
Within the time constraints of an office visit, primary care physicians are expected to address preventative health needs as well as chronic disease management, said Dr Lisa Kransdorf, an associate clinical professor of medicine at the Geffen School and a study co-author.
She said chronic disease management will often take priority.
“In cases where the patient has other providers such as specialists and clinical pharmacists actively involved in their chronic disease management, there is opportunity for primary care physicians to attend to preventative care gaps,” the researcher added:
There are some limitations to the findings.
The search yielded only 44 studies, many of which relied on patient recall, which can be unreliable, highlighting the need for further research.
In addition, most of the studies analysed had small sample sizes or were conducted at a single site, limiting how applicable the findings might be in other settings.

 Entrepreneur2 weeks ago
Entrepreneur2 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Ageing4 weeks ago
Ageing4 weeks agoCalifornia plans US$3.4m menopause care overhaul

 Menopause3 weeks ago
Menopause3 weeks agoWatchdog bans five ads for women’s heath claims

 Pregnancy2 weeks ago
Pregnancy2 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Menopause4 weeks ago
Menopause4 weeks agoMenopause has no lasting impact on cognition, research finds

 Entrepreneur3 weeks ago
Entrepreneur3 weeks agoWHIS USA 2026 announces first ticket release for landmark Women’s Health Innovation Summit

 News2 weeks ago
News2 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Entrepreneur3 weeks ago
Entrepreneur3 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up