News
Women in England “failed” by maternity services, says report
Significant changes need to be made to prevent more tragedies, England’s health ombudsman has warned
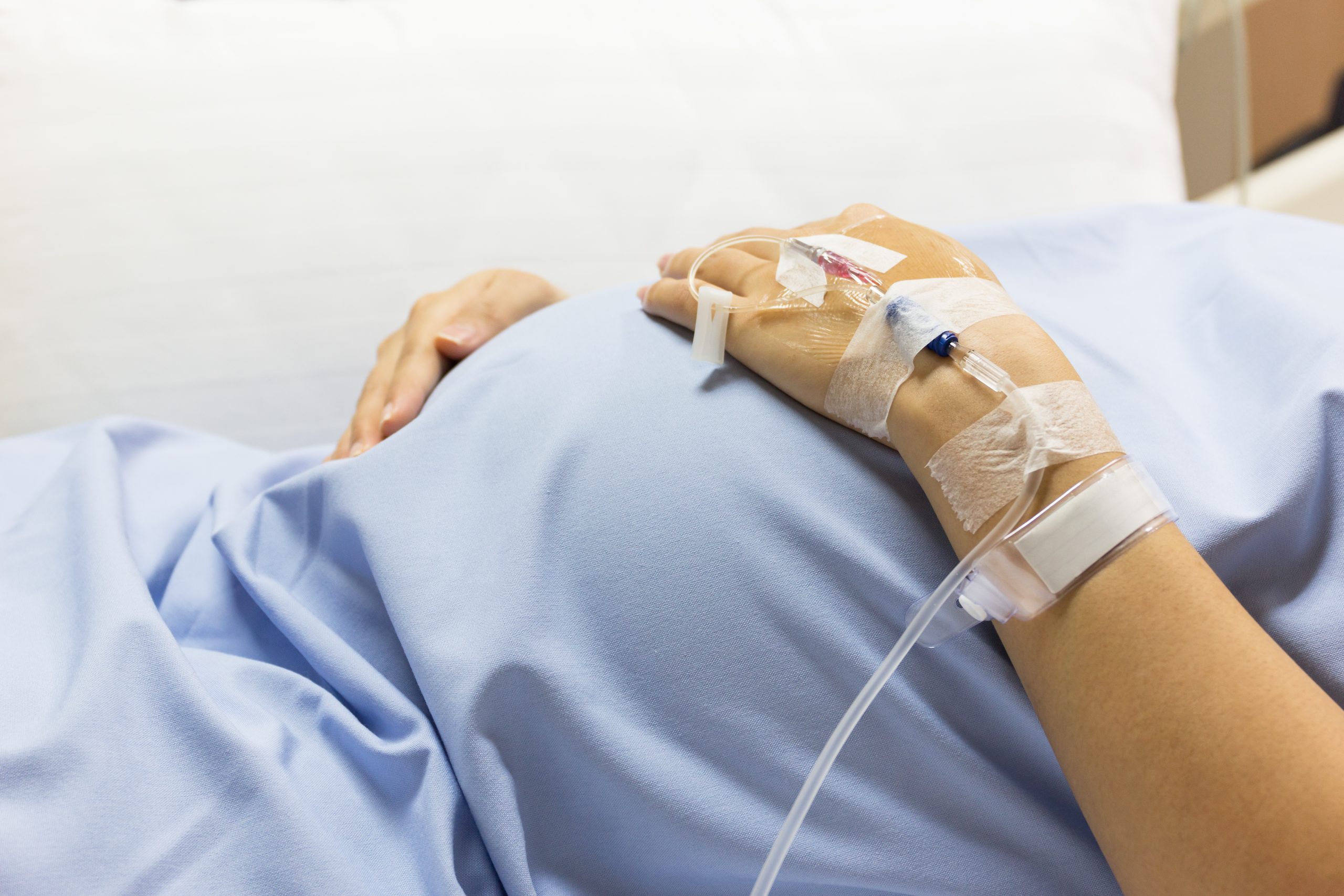
Too many women and babies are being put at risk as expectant and new parents are “repeatedly failed” by maternity services, England’s health ombudsman has said.
In a new report, the Parliamentary and Health Service Ombudsman has warned that despite a number of major reviews into maternity services, lessons are not being learned.
The report shines a spotlight on these failings by sharing the stories of women who have been affected by failures in maternity services.
It has found that repeated failings around communication, diagnosis, aftercare, and mental health support are still taking place, putting expectant and new mothers at risk.
One story shared in the report was from Patricia Michael who experienced bleeding during her pregnancy. No ultrasound scans were carried out to investigate the bleeding, the ombudsman has found
Staff also did not properly explain her delivery options or the induction of labour process.
After she had her baby, her placenta did not deliver naturally as it should. The placenta was removed manually, not in an operating theatre under anaesthetic, which meant a large part of it remained. This led to Patricia being in pain and needing two more operations to remove the rest of the placenta.
Staff did not explain or provide her with information about a haematoma on her baby’s head before she left the hospital which caused her distress.
“What happened to me should never be allowed to happen to anyone else,” said Patricia.
“It was a traumatic experience that affected me deeply and still does. All women should be able to trust the care they’re receiving is the best and that everything is being done as it should be.
“You should not be made to feel wrong when raising your own concerns. You know your own body. I hope that improvements are made so that no other woman has to go through what I did.”
The report also shares the story of Miss O, who was 21 weeks pregnant when she miscarried her daughter alone onto the hospital floor while in a labour ward.
PHSO found failings in the way her pain relief was managed, poor communication from staff about what to expect from a miscarriage at this stage of pregnancy and missed opportunities to check the progression of her miscarriage.
After Miss O left the hospital, the mortuary service failed to tell her the date of her daughter’s funeral, and the baby was buried without the family’s knowledge. The family were then given the wrong plot number for where their daughter was buried.
Parliamentary and Health Service Ombudsman, Rob Behrens, said: “These cases are extremely distressing. People should be able to trust that the care they receive during what should be one of the happiest times of their lives will be safe, effective, and compassionate.
“Sadly, this is often not the case. Failures in maternity care can have a devastating impact on women, their babies, and their families, and that impact can be long-lasting.
“Expectant and new parents are being failed right across the country, and very often in the same ways. The fact that we are still seeing the same mistakes over and over again shows that lessons are not being learned.
“This is unacceptable. There needs to be significant improvements and change.”
Complainants have told PHSO during the course of its investigations that they want to make sure their stories are heard.
“Everyone has the right to complain if they receive poor care,” Behrens added.
“I want to assure patients and families who have experienced something like this that their voice matters.
“One of the main reasons people come to the ombudsman is because they don’t want others to go through what happened to them.
“By sharing their experience, they can drive improvements to help stop mistakes happening again and make maternity services safer for everyone.”
Mental health
Lifting weights shows mental health and cognitive benefits in older women, study finds

Weightlifting can improve memory and mental health in older women, whether they lift heavier or lighter weights, a clinical trial has found.
The study suggests structured exercise could offer a non-drug way to help protect the ageing mind.
As people age, physical abilities often decline and the risk of cognitive impairment rises.
Women can also face a higher risk of depression and anxiety later in life because of menopause, hormonal changes and shifting social factors.
Over time, poor mental health can speed up physical and cognitive decline.
Medical professionals often recommend cardiovascular and resistance training to help preserve physical independence.
Beyond building muscle and strength, lifting weights may also help protect the brain.
The research team recruited 120 women with an average age of 68 who were not taking part in any structured exercise programmes.
Before the intervention, independent cardiologists screened the volunteers using diagnostic stress tests to make sure they could take part safely.
The researchers then divided the women into three equal groups based on their baseline physical strength to ensure a balanced comparison.
The first group followed a resistance training programme using heavier weights for eight to 12 repetitions.
The second performed the same exercises using slightly lighter weights for 10 to 15 repetitions. The third acted as a control group and remained sedentary throughout the trial.
For three months, the active groups visited the university fitness facility three mornings a week.
Under the direct supervision of qualified fitness experts, participants completed three sets of eight different full-body exercises. These included weight machines and free weights, with movements such as chest presses, leg extensions, seated rows and bicep curls.
As the women grew stronger over the 12 weeks, supervisors progressively increased the weight they lifted.
This ensured participants stayed within their assigned repetition range while maintaining proper breathing and movement technique. Researchers also told all participants not to start any new exercise outside the laboratory setting.
The scientists carried out a broad set of cognitive and psychological tests before the programme began and again shortly after it ended.
They used the Montreal Cognitive Assessment to measure spatial skills, short-term memory and language processing.
The team also used several standardised surveys to track symptoms of geriatric depression and general anxiety.
Other tests assessed executive function, the mental processes involved in planning, focusing attention and multitasking.
In the Trail Making Test, the women had to connect a scattered sequence of numbers and letters as quickly as possible to assess cognitive flexibility.
In another verbal test, they had to name as many words beginning with the letter F, or as many animals as possible, within 60 seconds.
The researchers also used a computerised Stroop test to assess inhibitory control. In this visual test, the women saw words such as “red” or “black” displayed in conflicting ink colours, such as green.
They had to suppress the automatic urge to read the word and instead press a button matching the ink colour.
After the three-month intervention, both groups of weightlifters showed clear improvements in their test scores.
Their performance on the overall cognitive assessment rose, and their reaction times in executive function tests fell substantially.
The control group showed no such improvements, and in some categories their mental performance worsened slightly.
The structured exercise also reduced the severity of mood disorders among the active participants.
Scores for depressive symptoms fell by roughly 34 per cent in the lower repetition group and 24 per cent in the higher repetition group. Anxiety scores fell by more than 40 per cent in both groups.
The researchers said these improvements met the threshold for a clinically meaningful difference.
In practical terms, that means the psychological benefits were large enough for the women to notice in their daily emotional state.
The trial found no major differences in outcomes between the two repetition strategies, suggesting both intensities worked equally well against cognitive decline.
The study has several caveats that may shape future research into the neurological benefits of structured exercise.
The testing relied heavily on self-reported psychological surveys, which can be affected by subjective bias or temporary changes in mood.
The team also did not closely track differences in the women’s light daily physical activity outside the gym.
The researchers also said the social structure of the fitness programme may have contributed to the emotional benefits.
For 12 weeks, the active participants exercised in a shared, supportive environment, with regular contact with peers and supervisors.
This kind of consistent social interaction can help reduce loneliness and provide psychological relief.
Future trials will need to isolate whether different exercise durations or extra social interaction change these positive neural effects.
Even so, the results suggest resistance training could offer an accessible way to help treat mild cognitive and mood problems.
Regular weightlifting may benefit the mind as well as the muscles in older adults.
Mental health
Poor mental health, poverty and pollution significantly raise women’s heart failure risk – study
Diagnosis
Women gaslit over hysteroscopy pain, Mumsnet posts reveal

Women have described being dismissed and left in serious pain during routine hysteroscopy examinations, with many given little or no pain relief.
Users of parenting forum Mumsnet who underwent hysteroscopy procedures also shared concerns about receiving unclear information before treatment and being given little or no pain relief afterwards.
Some women, who described feeling physically and emotionally vulnerable, compared the experience to sexual assault.
Research led by the University of Reading analysed 4,644 posts from Mumsnet users written between 2018 and 2024.
Susanne Cromme, lead author from the University of Reading, said: “Women in their thousands say they are going into hysteroscopy procedures unprepared, left in more pain than they were led to expect, and feeling that their experience is not being taken seriously, our analysis shows.
“This is not simply an online pile-on. The themes we found in our research are consistent with what clinical studies already tell us about hysteroscopy.
“But by listening to women talk to each other openly, without a researcher in the room, we get a much richer picture of the issues facing patients.”
The study was published following the launch of the Mumsnet campaign to End Medical Misogyny, which is fighting to end the “systemic dismissal, disbelief or de-prioritisation of women’s symptoms in healthcare”, and comes after health secretary Wes Streeting said the health system “too often gaslights women, treating their pain as an inconvenience.”
Justine Roberts, founder of Mumsnet and Gransnet, said: “This research makes clear that too many women are still experiencing severe pain during hysteroscopy, and that problem is compounded by unclear information, inconsistent pain relief and a lack of proper consent.
“These are not one-off failures, they form a repeated pattern and that’s exactly what Mumsnet’s medical misogyny campaign is highlighting: systemic failings in women’s healthcare.
“Nothing encapsulates that more clearly than the expectation that women should endure avoidable pain during gynaecological procedures. If the NHS is serious about tackling medical misogyny, this has to change.”
Around 71,000 hysteroscopy procedures take place every year in England.
According to the analysed Mumsnet posts, women were told procedures would be no worse than a smear test, felt unable to stop once they had started and found that the pain relief available depended entirely on which NHS trust they attended.
The analysis identified five recurring problems among hysteroscopy patients: not enough information before the procedure; women feeling exposed and unprotected; a “postcode lottery” for pain relief, with wide variation between trusts; pain being played down by staff; and an unequal standard of care.
Women also questioned why sedation routinely offered for procedures such as colonoscopies and endoscopies, which examine the bowel and digestive tract, was not available for gynaecological procedures.
The researchers said the findings suggest the problems go beyond individual clinicians, as the posts reflect wider structural issues in women’s healthcare, including potentially underfunded services and unequal standards of care.
The study calls for NHS trusts to introduce standardised consent processes that give women clear information about pain, alternatives and what to expect.
It also recommends consistent pain management protocols across all hospitals, and training for clinicians in trauma-informed care.

 Entrepreneur3 weeks ago
Entrepreneur3 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Menopause4 weeks ago
Menopause4 weeks agoCalifornia plans US$3.4m menopause care overhaul

 Pregnancy3 weeks ago
Pregnancy3 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Menopause4 weeks ago
Menopause4 weeks agoWatchdog bans five ads for women’s heath claims

 Entrepreneur4 weeks ago
Entrepreneur4 weeks agoWHIS USA 2026 announces first ticket release for landmark Women’s Health Innovation Summit

 Menopause4 weeks ago
Menopause4 weeks agoMenopause has no lasting impact on cognition, research finds

 News3 weeks ago
News3 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Opinion3 weeks ago
Opinion3 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up