News
Klinikk Hausken deploys Fairtility’s CHLOE technology, bringing transparent AI solution to Norway’s largest fertility network
Klinikk Hausken validated CHLOE technology on large data sets in two of its embryology labs prior to implementation
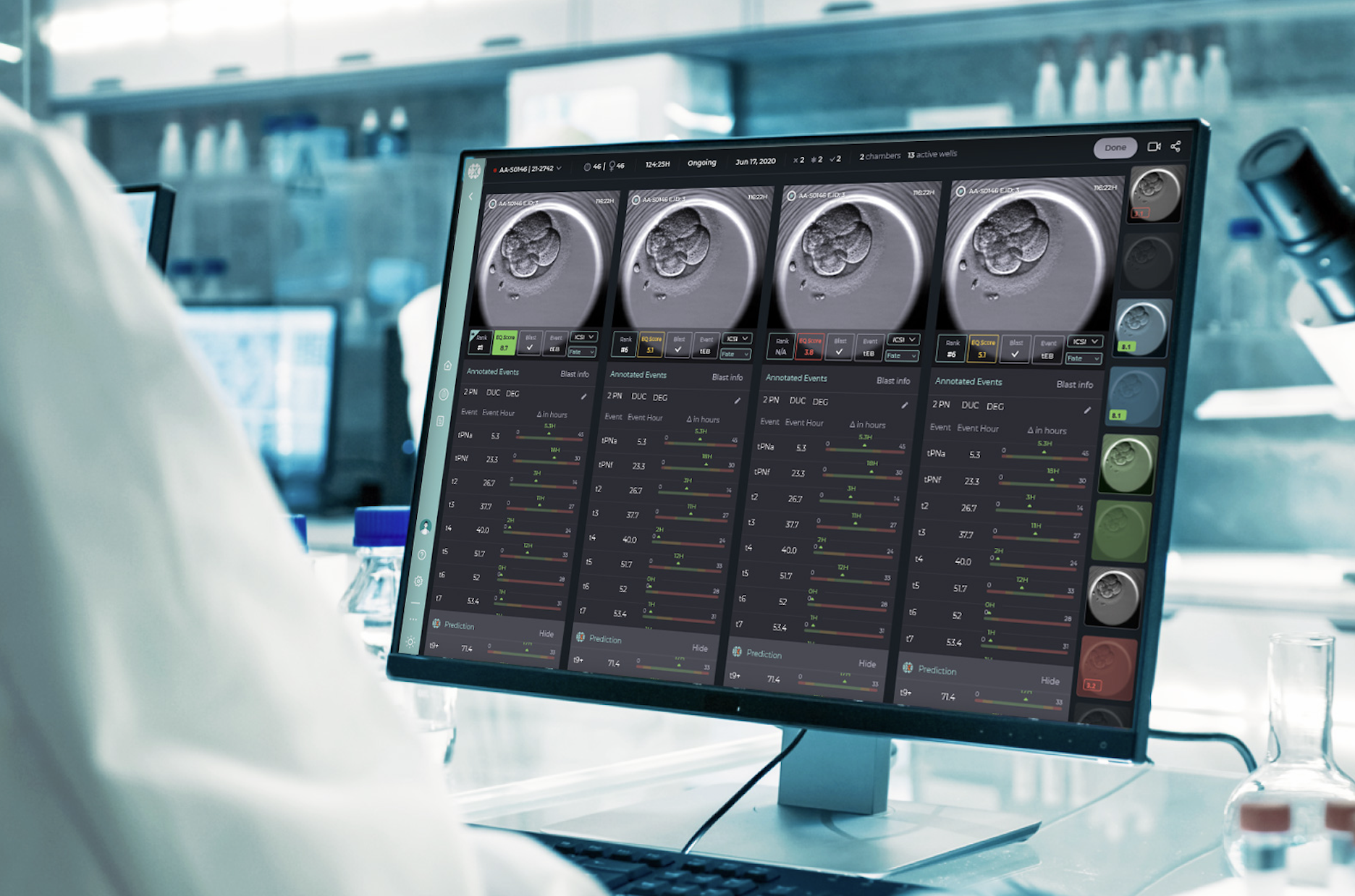
Fairtility, the transparent AI innovator powering reproductive care for improved outcomes, has announced that Klinikk Hausken, part of Medicover and Norway’s largest fertility network, has successfully deployed Fairtility’s CHLOE technology in all five of its embryology labs.
“We selected CHLOE EQ™ for its unmatched ability to provide quantifiable biological data on embryo development in language that our embryologists trust: human biology,” said said Shabana Sayed, senior embryologist and IVF lab manager at Klinikk Hausken, part of Medicover.
“Its transparency and interpretability set it apart from other AI-based decision support tools available.
“CHLOE EQ’s reliability and transparency have been instrumental in both our clinical and embryology teams wholeheartedly embracing AI technology in our routine workflow.
“Offering this transparency to both our internal teams and our patients is transformative to the IVF journey, which has historically been a ‘black box’ process.”
Klinikk Hausken validated CHLOE technology on large data sets in two of its embryology labs prior to implementation. Following this process, Norway’s largest fertility network implemented CHLOE technology into workflows across its clinics.
Despite utilising different time lapse incubator (TLI) systems in its various labs, CHLOE integration was seamless across TLIs and with the network’s electronic medical record system.
“CHLOE technology is bringing standardisation to the subjective and differentiated decision-making that takes place in embryology labs, where protocols and equipment may differ from lab to lab, and with embryologists having varying levels of experience,” explained Eran Eshed, co-founder and CEO of Fairtility.
“CHLOE EQ augments embryologists’ abilities and reduces their administrative time, essentially super-charging each embryologist to be more effective in the lab while reducing risk-factors for burnout.”
CHLOE EQ has augmented and standardised decision-making processes for selecting the most viable embryos for transfer or for cryopreservation.
It provides automated annotations of embryos’ biological development, including morphokinetic timings and provides accurate predictions for blastocyst development and expansion.
Supporting clinical decision-making and streamlining workflows has also resulted in operational benefits. Klinikk Hausken can now more efficiently schedule embryo transfers for patients at the optimal point in embryos’ development process.
Additionally, CHLOE EQ reports are utilised in daily treatment summary meetings with clinical and nursing staff, ensuring patients receive consistent, reliable and accurate information about their embryo quality.
Klinikk Hausken is Norway’s largest private IVF network, supporting over 1,500 IVF cycles annually. The network is committed to investing in its team and its technology, all to support improved patient care, as prospective parents pursue their dreams of having children.

Fertility
Toxins and climate harms having ‘alarming’ effect on fertility, research warns

Simultaneous exposure to toxic chemicals and climate-related heat may be worsening fertility harms across humans and wildlife, research suggests.
The review of scientific literature looks at how endocrine-disrupting chemicals, often found in plastic, together with climate-related effects such as heat stress, are each linked to lower fertility and fecundity, meaning the ability to reproduce, across species including humans, wildlife and invertebrates.
Though the reproductive harms of each issue in isolation are well studied, there is little research on what happens when living organisms are exposed to both.
“Together, the two issues are likely to pose a greater threat to fertility, and the additive effect is “alarming”, said Susanne Brander, a study lead author and courtesy faculty at Oregon State University.
“You’re not just getting exposed to one, but two, stressors at the same time that both may affect your fertility, and in turn the overall impact is going to be a bit worse,” Brander said.
The paper looked at 177 studies.
Shanna Swan, a co-author on the new paper, co-produced a 2017 study that found sperm levels among men in western countries had fallen by more than 50 per cent over four decades. Other research has suggested human fertility has been declining at a similar rate.
The University of Washington’s Institute for Health Metrics and Evaluation has previously said the world was approaching a “low-fertility future”, with more than three quarters of countries below replacement rate by 2050.
The new paper’s authors focused on the effects of endocrine-disrupting chemicals and substances, including microplastics, bisphenol, phthalates and PFAS.
These are thought to cause a range of serious reproductive problems, disrupt hormones and be a potential driver of falling fertility.
Brander said the harms linked to these chemicals are often similar across organisms, from invertebrates to humans.
Phthalates, for example, have been linked to altered sperm shape in invertebrates, spermatogenesis in rodents, meaning sperm production, and reduced sperm counts in humans.
PFAS are also thought to affect sperm quality, and both have been linked to hormone disruption.
The chemicals are widespread in consumer goods, so people are often regularly exposed.
Meanwhile, previous research has shown how rising temperatures, lower oxygen levels and heat stress, among other effects linked to climate change, may also worsen infertility.
Heat stress has been found to affect human hormones, and is linked to spermatogenesis in rodents and bulls.
Research shows temperature also plays a role in sex determination in fish, reptiles and amphibians.
The species has evolved to choose which sex it produces in part based on temperature, and the heating planet can “push it too far in one direction or the other, which overrides that evolutionary benefit”, Brander said.
Similarly, many endocrine disruptors may alter environmental sex determination.
The study set out some of the overlapping effects of chemical exposure and climate change across taxonomic groups, from invertebrates to humans.
In birds, for example, exposure to increased temperature, PFAS, organochlorines and pyrethroids may each individually cause abnormal sperm, increased fledgling mortality, abnormal testes and population decline.
“What happens if they’re exposed to more than one of those stressors at the same time? There has been little exploration of that question.
“Even if there have not been a lot of studies looking at these simultaneously, if you have two different factors that both cause the same adverse effect, then there’s a likelihood that they are going to be additive,” Brander said.
Katie Pelch, a senior scientist with the Natural Resources Defense Council nonprofit, who was not part of the study, said the authors had reviewed high-quality science.
She said she wanted to see more examples of the overlap in impacts, but agreed with the overall premise.
“It is likely [multiple stressors] would have an additive effect, at very least, even if they have different mechanisms of harm,” Pelch added.
The solution to the systemic problems would involve tackling climate change and reducing the use of toxic chemicals.
The study cites the global reduction in the use of DDT and PCBs achieved under the Stockholm Convention as an example of an effective measure, but Brander said much more is needed.
“There is enough evidence in both areas to act to reduce our impact on the planet,” she said.
Pregnancy
Home blood pressure checks could lower heart risks for new mothers – study
Fertility
Researcher explores weight loss jab impact on PCOS

 Events4 weeks ago
Events4 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Entrepreneur4 days ago
Entrepreneur4 days agoFuture Fertility raises Series A financing to scale AI tools redefining fertility care worldwide

 Pregnancy4 weeks ago
Pregnancy4 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Opinion4 weeks ago
Opinion4 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up

 News4 weeks ago
News4 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Fertility2 weeks ago
Fertility2 weeks agoFuture Fertility partners with Japan’s leading IVF provider, Kato Ladies Clinic

 Mental health6 days ago
Mental health6 days agoLifting weights shows mental health and cognitive benefits in older women, study finds

 Menopause2 weeks ago
Menopause2 weeks agoMore research needed to understand link between brain fog and menopause, expert says