News
Comment: Achieving culturally competent care
Gloria Kolb, co-founder and CEO of Elitone on addressing the unique needs of women from diverse backgrounds

Personalised medicine has gained a lot of attention as of late. It can mean suiting a treatment to the genetic makeup of the patient. In a broader sense, it means competent care that is not one-size-fits-all and more than acknowledges a patient’s background, but care that takes into account cultural identity, values, and health beliefs.
Especially in women’s health, women from different cultural, ethnic, and socioeconomic backgrounds often face unique health challenges and additional barriers that require culturally competent care.
In this ever-evolving field, and as medical innovations advance, practitioners must take the time to understand and respect each woman’s cultural differences that influence health behaviors, perceptions, and communication. This approach fosters trust and improves health outcomes by improving understanding and compliance with treatments. As we continue to innovate in women’s health, addressing these differences is crucial to bridging the gap between access and outcome disparities that have disproportionately affected women from diverse communities.
Understanding the unique needs of diverse women
Women from different cultural backgrounds often face distinct health challenges that are shaped by factors such as genetics, lifestyle, and societal expectations. These disparities highlight the importance of tailoring healthcare to meet the specific needs of each group.
The traditional “one-size-fits-all” approach in medicine does not account for the significant differences in how certain conditions manifest across various populations. Cultural identity is just one of many factors that shape an individual’s health needs and experiences. Within any given ethnic group, there is significant diversity in terms of lifestyle, socioeconomic status, education, and personal health beliefs.
Assumptions based solely on ethnicity can lead to stereotyping and the risk of overlooking personal nuances that are critical to effective healthcare. For example, while a Latina woman may statistically be at higher risk for diabetes, assuming that every Latina shares the same risk profile ignores the reality that individual behaviors, family history, and access to resources play crucial roles.
In another example, black women at one time were thought to have lower incidences of incontinence. Only after further research was conducted did it show that black women under-reported their conditions more than other races, and when black women did present with incontinence, their conditions were already much worse.
Regarding certain socio-economic statuses, prescribing weekly pelvic floor physical therapy or neurostimulation office visits has led to poor compliance. Often, these women can’t hire a babysitter for every office visit or take time off from work in the middle of the day. Poor compliance is often simply due to a lack of transportation.
Healthcare providers must balance recognising common trends within ethnic groups and treating each patient as an individual with unique circumstances. This approach not only builds trust but also allows for more effective diagnosis and treatment, as patients are more likely to feel heard, engage in open communication, and collaborate in their healthcare when they feel understood on a personal level.
The role of healthcare providers in culturally competent care
Healthcare providers play a crucial role in delivering culturally competent care by actively educating themselves about the communities they serve. This includes being aware of the social determinants of health — factors such as income, education, and environment — that disproportionately affect women from marginalized communities.
It’s understood that healthcare providers are woefully busy. On average, OBGYNs spend about 13 minutes with each patient to understand issues, examine them, and give diagnoses and treatments. During this time, women, as family health caretakers, may bring up issues other than their own.
Cultural differences can influence their perceptions of illness and treatment, delay decisions until the family is included, or avoid needed taboo topics such as pelvic, mental, and sexual health. Providers who are sensitive to these nuances can navigate conversations with empathy and respect, leading to better communication and patient adherence to treatment plans.
Innovative approaches to culturally competent care
Innovation in healthcare is not only about developing new treatments or technologies but also about rethinking how care is delivered to ensure it meets the needs of diverse populations. One promising approach is integrating community health workers (CHWs) into healthcare teams. CHWs are often members of the communities they serve, making them well-positioned to provide culturally relevant health education, support, and advocacy.
Another innovative solution is using telemedicine to reach women in underserved areas. Telemedicine allows healthcare providers to connect with patients who may face geographical, financial, or even social barriers to in-person, mid-day care.
For women from rural or immigrant communities, telemedicine offers a way to access culturally competent care from providers who may not be physically accessible. Lower-paid workers often have jobs that are more inflexible regarding taking time off during work time. By breaking down these barriers, telemedicine can help bridge the gap between diverse populations and quality healthcare.
Additionally, healthcare institutions can leverage technology to create tailored health education materials in multiple languages and formats. Digital platforms that deliver culturally specific content about preventive care, maternal health, and chronic disease management can empower women from different backgrounds to take control of their health.
Similarly, at-home treatments can allow for easier treatments on your own time without taking transportation time or time off from work.
The future of culturally competent care in women’s health
The demand for culturally competent care in women’s health will only grow as the population does. Yet, the future of healthcare cannot rest solely on broad generalizations about ethnicity or culture.
Ultimately, the future of culturally competent care in women’s health lies in moving away from a one-size-fits-all model and embracing a patient-centered approach that respects each woman’s unique combination of cultural, social, and personal factors.
By doing so, healthcare providers can ensure that women from all backgrounds receive the quality care they deserve, leading to improved health outcomes and a more equitable healthcare system.
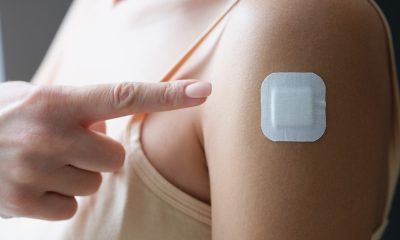
Gloria Kolb is the CEO and co-founder of Elitone, the first non-invasive, FDA-cleared, wearable treatment for women with urinary incontinence. Elitone’s accolades include winning Best New Product by My Face My Body, Sling Shot 2020, finalist in the Women Startup Challenge, and many startup pitch competitions. As an inventor with 30+ patents, Gloria has been featured in Forbes as a Top Scientist Driving Innovation in Women’s Health. Her creative designs and problem-solving abilities have earned her recognition, such as Boston’s “40 Under 40” and MIT Review’s “World’s Top Innovators under 35.” She has engineering degrees from MIT and Stanford, as well as an MBA in entrepreneurship from Babson College.
Diagnosis
Researchers teach AI to spot cancer risk by squeezing individual breast cells
Diagnosis
Experimental drug drowns triple-negative breast cancer cells in toxic fats

An experimental drug slowed triple-negative breast cancer in mice by flooding tumour cells with toxic fats.
Triple-negative breast cancer lacks three common drug targets, making it one of the hardest-to-treat and most aggressive forms of the disease.
The compound, known as DH20931, appears to push cancer cells past their limits by triggering a surge in ceramides, fat-like molecules that place the cells under intense stress until they self-destruct.
In lab experiments, the drug also made standard chemotherapy more effective. When combined with doxorubicin, researchers were able to reduce the dose needed to kill cancer cells by about fivefold.
The drug targets an enzyme known as CerS2 to sharply increase production of these lipids and stress cancer cells. Healthy cells, by contrast, showed lower sensitivity to the drug in lab tests.
While the early results are promising, further preclinical and clinical trials would still be needed to determine the safety and effectiveness of DH20931 in humans.
Satya Narayan, a professor in the University of Florida’s College of Medicine, led the study with an international group of collaborators.
The researchers published their results on human-derived tumours on 21 April and presented their findings on combination therapy at the annual meeting of the American Association for Cancer Research in San Diego.
Narayan likened the drug’s effects to a home’s electrical system handling a power surge.
While healthy cells act like a properly grounded and installed circuit, cancer cells are more like a jumble of mismatched wires and faulty fuses. DH20931 overwhelms cells not with electricity, but with fats.
He said: “When that surge goes into the cancer cells, they cannot handle the amount of power they are getting. The fuses burn out, the cell can’t handle the surge and it dies.”
The compound was developed at the University of Florida in the lab of Sukwong Hong.
Hong, now a professor at the Gwangju Institute of Science and Technology in South Korea, created DH20931 as one of many drug candidates tested for efficacy in Narayan’s lab.
In the study, researchers implanted human triple-negative breast cancer tumours into mice and treated them with DH20931.
The drug significantly slowed tumour growth without causing noticeable weight loss or signs of toxicity in the animals. In separate lab experiments, it also showed activity against other breast cancer subtypes.
In addition to increasing lipid levels, DH20931 triggers a second stress signal by flooding cells with calcium.
Together, these effects disrupt the mitochondria, the structures that produce a cell’s energy, ultimately leading to cell death.
Narayan said: “It does not just follow one pathway but it goes through multiple pathways. It’s a two-hit hypothesis.
“These pathways are common in all breast cancer types and other solid tumours, so we think this drug can be useful not only in triple-negative breast cancer but potentially other cancers as well.”
Fertility
Future Fertility raises Series A financing to scale AI tools redefining fertility care worldwide

Future Fertility Inc. has announced the closing of a US$4.1 million Series A financing round.
The round was led by M Ventures (the corporate venture capital arm of Merck KGaA, Darmstadt, Germany) and Whitecap Venture Partners, with participation from new investors Sandpiper Ventures, Gaingels, and Jolt VC.
The financing will accelerate Future Fertility’s commercial expansion into Asia-Pacific and support its entry into the United States, including planned FDA 510(k) clearance for additional products as part of a broader U.S. market entry strategy.
Proceeds will also advance the development of a broader AI platform, from egg assessment through to embryo transfer, designed to support clinicians, embryologists, and patients across the full IVF journey.
M Ventures and Whitecap have supported Future Fertility’s mission to translate AI innovation into meaningful clinical outcomes since the company’s earliest stages.
Oliver Hardick, investment director, M Ventures, said: “Future Fertility is addressing a critical unmet need in reproductive medicine with a differentiated AI platform grounded in clinical data and real-world workflow integration.
“We are excited to continue supporting the company and team because we believe its technology has the potential to improve decision-making for clinicians, bring greater clarity to patients, and help advance a more personalised standard of care in fertility treatment.”
Future Fertility’s AI platform addresses a long-standing gap in fertility care: historically, there has been no objective, clinically validated method for assessing egg quality (Gardner et al., 2025), despite it being one of the most important drivers of reproductive success.
The company’s suite of deep learning tools includes VIOLET™, MAGENTA™, and ROSE™, purpose-built for egg freezing, IVF, and egg donation respectively.
The tools are based on AI models trained and validated on more than 650,000 oocyte images and are deployed in over 300 clinics across 35 countries.
Rhiannon Davies, founding and managing partner, Sandpiper Ventures, said: “The best outcomes in fertility care globally come from better data and smarter tools. Future Fertility understands that, and they’ve built a platform that delivers on it.
“Sandpiper is proud to back a team turning rigorous science into real results for patients and clinicians alike.”
Partnerships with the world’s leading fertility networks – including IVI RMA and Eugin Group across Latin America and Europe, FertGroup Medicina Reproductiva in Brazil, and most recently announced Kato Ladies Clinic in Japan – reflect growing demand for objective, AI-powered oocyte assessment in fertility care. In the United States, ROSE™ is newly available under an FDA 513(g) determination.
Research shows that approximately 50 per cent of IVF patients do not understand their likelihood of success, and many discontinue treatment prematurely, even though cumulative success rates improve significantly with multiple cycles (McMahon et al., 2024).
By delivering earlier clarity on egg quality, Future Fertility’s tools support more informed conversations between clinicians and patients, helping set realistic expectations and guide decisions about next steps.
Future Fertility’s growing evidence base spans seven peer-reviewed publications in Human Reproduction, Reproductive BioMedicine Online, Fertility & Sterility, and Nature’s Scientific Reports, and more than 70 scientific abstracts accepted and presented with partner clinics at conferences worldwide.
Christine Prada, CEO, Future Fertility, said: “Fertility treatment is one of the most emotionally and physically demanding experiences a person can go through.
“Every patient deserves objective data, not just a best guess, to support better decisions at critical moments in their care.
“This funding means we can bring that clarity to more patients, in more countries, at a moment when it matters most.”
Find out more about Future Fertility at futurefertility.com

 Entrepreneur3 weeks ago
Entrepreneur3 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Fertility3 days ago
Fertility3 days agoFuture Fertility raises Series A financing to scale AI tools redefining fertility care worldwide

 Pregnancy4 weeks ago
Pregnancy4 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 News3 weeks ago
News3 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Opinion4 weeks ago
Opinion4 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up

 Mental health2 weeks ago
Mental health2 weeks agoMore research needed to understand link between brain fog and menopause, expert says

 Fertility2 weeks ago
Fertility2 weeks agoFuture Fertility partners with Japan’s leading IVF provider, Kato Ladies Clinic

 News2 weeks ago
News2 weeks agoSelf-employment linked to better cardiovascular health outcomes in Hispanic women

























2 Comments