Diagnosis
Woman files lawsuit claiming fertility clinic ‘bootcamp’ caused her stroke

A London executive is suing a fertility clinic, alleging its IVF treatment led to her suffering a stroke.
Navkiran Dhillon-Byrne, 51, began private IVF treatment at the Assisted Reproduction and Gynaecology Centre (ARGC) in Wimpole Street, London, in April 2018.
Ten days after her treatment ended, on 28 April 2018, she suffered a stroke, which her lawyers say has left her with ongoing vision problems.
Ms Dhillon-Byrne is now suing the clinic and its head, Mohamed Taranissi, for negligence and breach of duty, saying medics failed to give her sufficient warnings about stroke risks linked to IVIg immunotherapy (intravenous immunoglobulin) – a one-off add-on treatment designed to moderate the body’s immune responses during pregnancy.
The clinic and Dr Taranissi deny liability, saying Ms Dhillon-Byrne was fully informed of the risks.
They also dispute that IVIg caused her stroke.
Central London County Court heard that Ms Dhillon-Byrne, chief marketing officer at the City of London base of an international software company, turned to private treatment after the NHS was unable to fund her IVF in 2014.
She had an unsuccessful attempt at another London clinic before choosing ARGC. She told the court she had been trying to have a child since 2014.
She said she selected ARGC after a friend recommended it, praising what they described as high success rates.
The clinic’s website describes its approach as “IVF boot camp” and promotes “in-depth investigations, daily monitoring and real-time treatment adjustments.”
Ms Dhillon-Byrne says she was not warned of the “specific” risks of thrombosis – blood clotting that can lead to stroke – in relation to the IVIg therapy.
She also says the clinic overstated her chances of success and failed to secure her “informed consent” before treatment began.
She argues that, had she been given a clear picture of her chance of a successful pregnancy, she would not have consented to IVF and the supplemental IVIg therapy.
Denying Ms Dhillon-Byrne’s claims, the clinic’s KC, Clodagh Bradley, told the court that the success rate advice given was “accurate and in accordance with the ARGC data.”
She added that Ms Dhillon-Byrne had been informed that the immune treatment was new and “still controversial.”
Lawyers said outside court that, if successful, Ms Dhillon-Byrne’s claim is likely to be worth “millions” due to the impact of the stroke on her high-flying career.
The trial continues.
Diagnosis
Women with osteoporosis face increased Alzheimer’s risk, study suggests

Women with osteoporosis may be more likely to carry a gene linked to Alzheimer’s, according to new research.
Scientists found that APOE4, the most common genetic risk factor for Alzheimer’s, can weaken bone quality in women, even when standard scans appear normal.
The study, carried out by researchers at the Buck Institute for Research on Ageing in California, US, and UC San Francisco, suggests the gene may damage bone at a microscopic level long before any visible signs.
These changes can emerge as early as midlife and remain invisible to routine imaging tests used to assess bone strength.
The findings suggest a link between Alzheimer’s risk and skeletal health and could help pave the way for earlier detection of both conditions.
Professor Birgit Schilling, a senior author of the study, said: “What makes this finding so striking is that bone quality is being compromised at a molecular level that a standard bone scan simply will not catch.
“APOE4 is quietly disrupting the very cells responsible for keeping bone strong – and it is doing this specifically in females, which mirrors what we see with Alzheimer’s disease risk.”
Doctors have long observed that people with Alzheimer’s suffer higher rates of bone fractures, while osteoporosis in women is known to be one of the earliest predictors of the disease.
Now scientists believe they may have uncovered why.
Researchers led by Dr Charles Schurman carried out a detailed analysis of proteins in aged mouse bone and found that tissue was unusually rich in molecules linked to neurological disease, including those associated with Alzheimer’s.
In particular, long-lived bone cells known as osteocytes showed elevated levels of APOE, with levels twice as high in older female mice compared with younger or male animals.
Further experiments using genetically modified mice revealed that APOE4 had a strong and sex-specific impact on both bone and brain tissue.
The disruption at the protein level was even greater in bone than in the brain.
However, the bone structure itself appeared completely normal under scans.
Instead, the gene interfered with a key maintenance process inside bone cells, preventing them from repairing microscopic channels that keep bones strong and resilient.
When this process breaks down, bones become more fragile even if they look healthy on standard imaging.
These results suggest bone cells could potentially act as early biological warning signs of cognitive decline in women carrying APOE4.
Professor Lisa Ellerby, another senior author, said: “We think targeting these cells may open a new front in preserving bone quality in this population.”
Experts say the findings highlight the need to view the body as an interconnected system rather than treating diseases in isolation.
Dementia, of which Alzheimer’s is the most common form, remains one of the UK’s biggest health challenges.
Around 900,000 people are currently living with the condition, a figure expected to rise to 1.6 million by 2040.
It is already the leading cause of death, responsible for more than 74,000 deaths each year.
Fertility
Future Fertility partners with Japan’s leading IVF provider, Kato Ladies Clinic

Future Fertility, a Toronto-based health technology company specialising in AI-powered fertility insights, has entered the Japanese market through a new commercial partnership with Kato Ladies Clinic — a globally recognised leader in IVF research and advancing clinical fertility care.
The collaboration marks Future Fertility’s first partnership in Japan and reflects growing global demand for technologies that bring greater objectivity and personalisation to fertility care.
Kato Ladies Clinic will integrate the company’s AI-powered oocyte (egg) quality assessment tools into its clinical workflows, with the aim of supporting more informed treatment planning and patient counselling across IVF and egg freezing cycles.
“At Kato Ladies Clinic, we are committed to advancing fertility care through innovation while maintaining a strong focus on individualised, patient-centred treatment,” said Keiichi Kato, chief executive officer.
“Partnering with Future Fertility enables us to integrate objective, data-driven insights into our clinical approach and better support our patients in making informed decisions.”
Future Fertility’s platform analyses images of oocytes using artificial intelligence trained and validated on a dataset of more than 650,000 unique oocyte images.
The technology is already in use at more than 300 clinics across more than 35 countries, helping clinicians better understand the developmental potential of individual eggs and provide patients with more personalised insight earlier in their treatment journey.
From Research Collaboration to Clinical Adoption
The partnership between Future Fertility and Kato Ladies Clinic began as a scientific research collaboration in 2024, marking the first use of AI-powered oocyte quality assessment in Japan.
The collaboration not only validated the technology in a new patient population and across diverse clinical protocols — including minimal stimulation cycles —but also resulted in a peer-reviewed publication in Reproductive BioMedicine Online (RBMO) and a poster abstract presentation at ESHRE 2025.
The joint research explored how AI-derived oocyte quality scores relate to early embryonic development and overall treatment outcomes. In a retrospective study conducted at Kato Ladies Clinic, researchers analysed nearly 2,800 mature oocytes across more than 1,300 ICSI cycles, linking image-based assessments of egg quality to key developmental milestones.
The study demonstrated that lower AI scores were associated with reduced fertilization rates, delays, and abnormalities in early embryo development, increased developmental errors, and lower-quality blastocyst formation.
Notably, the researchers also found that cumulative oocyte scores were a stronger predictor of live birth outcomes than the number of eggs retrieved — underscoring the importance of assessing egg quality alongside quantity.
“Our collaboration with Future Fertility has demonstrated how artificial intelligence can uncover meaningful biological differences between oocytes that were previously difficult to quantify,” said Kenji Ezoe, senior scientist.
“Bringing this technology into routine clinical use is an important step toward translating research into improved patient outcomes.”
Future Fertility’s VP of clinical embryology & scientific operations, Jullin Fjeldstad, noted that the findings provide important clinical validation.
“Our joint research with Kato Ladies Clinic has shown how AI-based oocyte assessment can be directly linked to numerous embryo development outcomes, from fertilization through early developmental milestones and blastocyst formation,” she said.
“We are excited to see this work translated into clinical practice.”
Growing Demand for Fertility Care in Japan
The partnership comes at a time when demand for fertility treatment in Japan continues to rise.
The country performs over 450,000 fertility treatment cycles annually, making it one of the largest markets globally. Delayed childbearing and evolving societal trends have also contributed to increasing interest in egg freezing.
As patients seek more clarity and personalization in their care, tools that provide earlier insight into reproductive potential are gaining traction.
“Entering the Japanese market with a partner like Kato Ladies Clinic is a significant step forward for our global commercial strategy,” said Rafael Gonzalez, Future Fertility’s VP of global sales & strategy.
“It reflects the growing demand for technologies that support more transparent, data-driven fertility care across diverse healthcare systems.”
Expanding a Global Footprint
Founded in 1993, Kato Ladies Clinic is known for its pioneering work in natural and minimal stimulation IVF and has long been a leader in clinical innovation in Japan.
For Future Fertility, the partnership represents both a geographic expansion and a continuation of its broader mission to bring AI-driven insights into routine fertility care.
“We are proud to partner with Kato Ladies Clinic, a globally respected leader in IVF and a pioneer in reproductive medicine in Japan,” said Future Fertility’s CEO, Christy Prada.
“This partnership represents an important milestone as we expand into Asia and continue our mission to bring objective, personalised insights into fertility care worldwide.”
Future Fertility develops AI-powered tools designed to generate personalised insights across the fertility journey.
Its flagship oocyte assessment technologies analyse egg images to provide objective, individualised measures of egg quality, supporting treatment planning, patient counselling, and clinical decision-making in egg freezing and IVF, while also enabling more data-driven approaches to donor egg distribution and quality assurance.
As fertility care continues to evolve, collaborations like this one are helping shape a new standard — one that emphasises earlier insight, greater transparency, and more personalised decision-making for patients navigating increasingly complex reproductive journeys.
Diagnosis
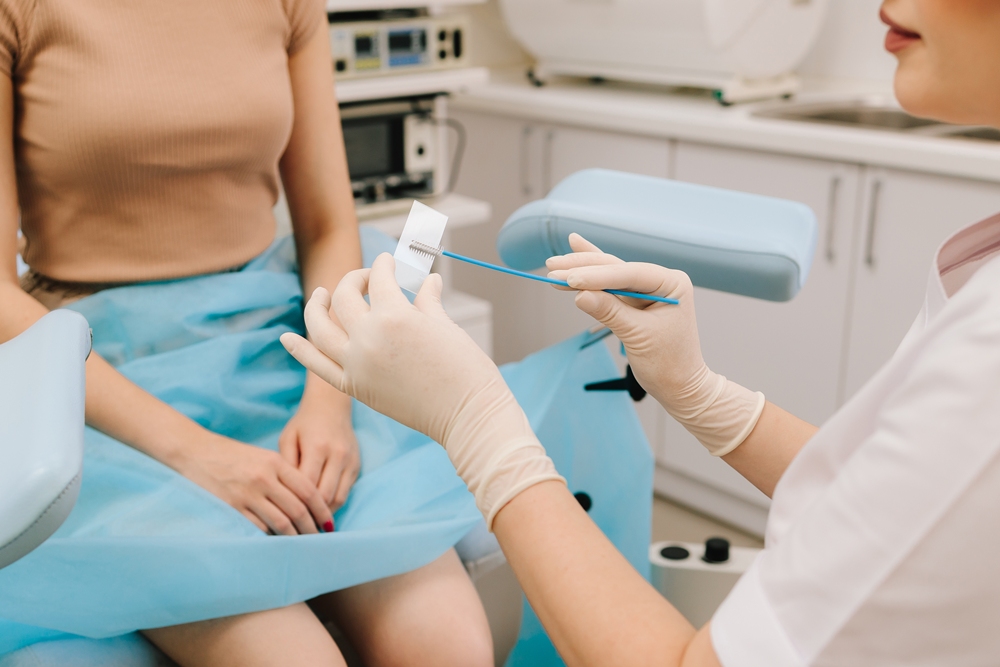
Smear test: Everything you need to know before your appointment
Article produced in association with Spital Clinic
Cervical screening saves thousands of lives from cervical cancer in the UK every year.
The programme has changed significantly in recent years, and understanding what it now involves — and what your results actually mean — is probably the most useful preparation you can do before your appointment.
Why Cervical Screening Exists — and What Changed in 2025
The NHS cervical screening programme now uses HPV primary screening — a method NHS England describes as testing for the human papillomavirus (HPV) rather than looking directly for abnormal cells.
If HPV is not found, the sample is not examined further; if HPV is found, the same sample is then checked for cell changes.
The reason HPV sits at the centre of this approach is straightforward. Nearly all cervical cancers are caused by certain high-risk types of HPV — and HPV is extremely common.
Most people encounter some form of it during their lives, and the body usually clears it without any treatment.
The problem arises when high-risk HPV persists, because over time it can cause cell changes in the cervix that, if left undetected, may eventually develop into cancer.
Cervical screening is therefore a prevention test, not a cancer diagnosis. Its purpose is to find those cell changes early, when treatment is straightforward and effective.
A significant change took effect in England on 1 July 2025.
The screening interval for those aged 25–49 was extended from three years to five years, in line with the 50–64 age group — so everyone aged 25 to 64 in England is now invited every five years.
The interval in Northern Ireland currently differs; Cancer Research UK has current details.
Who Is Invited and How to Book
NHS England invites everyone with a cervix aged 25 to 64, with the first letter usually arriving a few months before a person’s 25th birthday.
Invitations are sent automatically and are linked to GP registration — the simplest way to make sure yours arrives is to be registered with a GP and keep your contact details up to date. If your invitation hasn’t come through, any GP surgery can arrange an appointment.
Trans men and non-binary people registered as female with their GP will receive invitations automatically.
Those registered as male will not — but can self-refer through the NHS cervical screening programme website or ask their GP to arrange a test.
People over 65 are not routinely invited but are not excluded.
Anyone who has never been screened, or whose most recent result was abnormal, can request screening through their GP or a clinic.
Appointments are most commonly offered at GP surgeries, carried out by a nurse or doctor.
For those who prefer a different setting, shorter waits, or an appointment outside NHS hours, a private smear test can be arranged through specialist gynaecology clinics, often within a few days.
What Happens at a Smear Test Appointment
The test itself takes less than five minutes, with the full appointment lasting around ten minutes.
Knowing what happens — step by step — removes most of the uncertainty that makes it feel more daunting than it actually is.
You undress from the waist down and lie on an examination table, knees bent and falling gently apart.
The nurse or doctor applies a little lubricant and gently inserts a small speculum, which is opened just enough to make the cervix visible.
A small, soft brush sweeps a cell sample from the surface of the cervix. The speculum is removed, and you get dressed.
That is the entirety of the test.
A little preparation helps both comfort and sample quality.
Avoid vaginal medicines, lubricants, and creams for at least two days beforehand, as residue can interfere with the results. Avoid scheduling during your period for the same reason.
Loose-fitting clothing — a skirt or wide-leg trousers — makes undressing and repositioning much easier.
If you are going through the menopause, vaginal dryness can make speculum insertion uncomfortable.
Cancer Research UK notes that using a short course of oestrogen cream or pessaries for around two weeks beforehand can help considerably — though stop two days before the appointment to avoid affecting the sample.
It is worth mentioning to your GP when you book.
Most people feel some pressure or mild discomfort, but it does not usually hurt.
If you find it painful, you can ask for a smaller speculum, insert it yourself, or try lying on your side — all are standard adjustments. Light spotting afterwards is normal and usually clears within a few hours. You can ask to stop at any point.
Understanding Your Results
The most common result — received by 87 in every 100 people screened — is HPV not found.
That means no high-risk HPV was detected, your risk of developing cervical cancer before the next screen is very low, and nothing further is needed until your next invitation arrives in five years.
The other results fall into two categories. Nine in every 100 people are told HPV was found, but no cell changes were detected.
This is not a cancer result and does not require immediate treatment — it means high-risk HPV is present and the cervix is being monitored.
The pathway is a repeat screen at one year; if HPV is still present, another repeat at two years. Only if it persists at that point is a colposcopy referral made.
Four in every 100 people receive an HPV-positive result alongside detected cell changes, and are referred directly for colposcopy.
That referral is not a diagnosis of cancer.
A colposcopy is a closer examination of the cervix, carried out in a clinic using a magnifying device, allowing a clinician to look in detail at any flagged cell changes.
Most people who attend colposcopy do not have cervical cancer — NHS England is clear on this. If a biopsy is taken or cells are removed, there is a small risk of bleeding and infection, both well-managed.
Those who prefer not to wait for an NHS appointment can access a private colposcopy at specialist clinics.
Results usually arrive by post or through the NHS App within two to six weeks. Samples are kept for ten years.
HPV can remain in the body for many years without symptoms, so a positive result says nothing about recent exposure or transmission history.
HPV, the Vaccine, and When to See a GP Without Waiting
Nearly all cases of cervical cancer are linked to high-risk HPV.
The virus spreads through skin-to-skin genital contact, vaginal, anal or oral sex, and sharing sex toys — it does not require penetrative sex to pass between people. The vast majority of people who carry it clear it naturally and will never know they had it.
The UK’s HPV vaccination programme, which began in 2008, has meaningfully reduced risk in younger age groups.
But vaccinated people still need to attend cervical screening — the vaccine does not protect against all high-risk HPV types. Vaccination and screening work together; one does not replace the other.
Cervical screening runs on a schedule, but some symptoms need attention straight away — do not wait for your routine invitation.
According to NHS England, these include unusual vaginal bleeding, bleeding after sex, bleeding during or after the menopause, heavier periods than usual, changes in vaginal discharge, pain during sex, or persistent lower back or pelvic pain.
These symptoms do not confirm anything, but they need investigating without delay.
Attending every invitation remains the single most important thing anyone in the eligible age group can do — and with the 2025 extension to five-year intervals, each appointment now covers a longer window than it once did.
The extension of the English screening interval to five years is backed by strong evidence about the accuracy of HPV primary screening.
Simply turning up remains, by some margin, the most protective thing anyone in the eligible age group can do.
This article is for informational purposes only and does not constitute medical advice. For personal health concerns, consult a qualified healthcare professional. Cervical screening eligibility and intervals may vary; refer to current NHS guidance or your GP for the most up-to-date information applicable to your circumstances. This piece was produced in association with Spital Clinic, which provided background clinical information for editorial purposes. Hyperlinks to external sources are included for reference only and do not represent an endorsement of any product, service or organisation.

 Entrepreneur2 weeks ago
Entrepreneur2 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Menopause4 weeks ago
Menopause4 weeks agoCalifornia plans US$3.4m menopause care overhaul

 Menopause3 weeks ago
Menopause3 weeks agoWatchdog bans five ads for women’s heath claims

 Pregnancy2 weeks ago
Pregnancy2 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Entrepreneur3 weeks ago
Entrepreneur3 weeks agoWHIS USA 2026 announces first ticket release for landmark Women’s Health Innovation Summit

 Menopause4 weeks ago
Menopause4 weeks agoMenopause has no lasting impact on cognition, research finds

 News2 weeks ago
News2 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Entrepreneur3 weeks ago
Entrepreneur3 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up



























3 Comments