Menopause
Everything you need to know about hot flashes and nausea

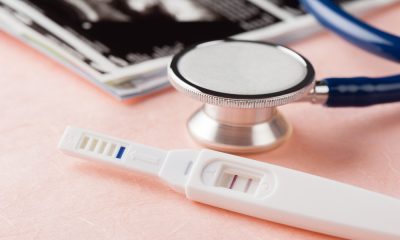
About 75 per cent of women experience hot flashes but many questions remain unanswered about the nausea that comes with it. Can hot flashes cause nausea? How? What to do?
A hot flash is a sudden feeling of warmth in the upper body, which is usually most intense over the face, neck and chest.
Hot flashes are the most common of an array of indicators of menopause and perimenopause called vasomotor symptoms.
They start when blood vessels near the skin’s surface widen to cool off, making you break out in a sweat. Some women have a rapid heart rate or chills too.
Can hot flashes cause nausea?
Yes, they can.
Hot flashes that occur at night can cause drenching night swears and, sometimes, they may be so strong that they can make the individual feel nauseous.
Other symptoms of hot flashes include headaches and migraines which may also cause nausea.
A menopausal woman can feel nauseous before, during or after a hot flash.
What causes nausea?
Suddenly feeling hot and nauseous with a hot flash is believed to be due to abrupt changes in serotonin, which can stimulate the area postrema, a part of the brain that controls nausea and vomiting.
Area postrema is located right next to the hypothalamus – the part of the brain that regulates temperatures. Due to hormonal fluctuations, the hypothalamus incorrectly detects that the body is overheating, and heat loss mechanisms are triggers, provoking a hot flash.
Nausea can also be caused by a sudden dip in blood pressure, by pressure on the liver or by blood sugar levels.
How to prevent nausea?
Treatments for nausea and hot flashes may involve a combination of lifestyle or dietary changes, along with prescription medications to help address the underlying causes.
A dietary change is one of the main lifestyle changes needed to reduce the risk of nausea during menopause. Menopausal women may want to avoid or decrease the consumption of alcohol, spicy foods, hot foods, hot beverages and caffeinated drinks.
Exercise, not smoking and reduced stress are also part of these lifestyle changes.
If the symptoms do not improve with lifestyle changes after three months, a doctor may recommend medications. These include HRT, oral contraceptive and selective serotonin reuptake inhibitors (SSRIs), a type of antidepressants.
To receive the Femtech World newsletter, sign up here.
Menopause
More research needed to understand link between brain fog and menopause, expert says

Brain fog in menopause is common but still poorly understood, with researchers calling for more work to explain the link and how best to support women.
For a new perspective article published in The Lancet Obstetrics, Gynaecology, & Women’s Health, researchers based in the UK and Australia reviewed the evidence on menopause-related cognitive symptoms. They found that symptoms such as forgetfulness, reduced concentration and brain fog are common during the menopause transition, but are still poorly recognised and under-researched.
More than two-thirds of women report difficulties with memory or concentration over the menopause transition. Multiple factors may contribute to these cognitive symptoms, including hormonal changes, sleep disturbances and psychological and psychosocial stress. Yet, because cognitive symptoms are not widely discussed, they can cause considerable worry, with some fearing they are signs of dementia or undiagnosed neurodevelopmental conditions.
The review paper emphasises that overall cognitive performance for women experiencing menopause-related brain fog typically remains within expected ranges and, importantly, that cognitive symptoms are not linked to an increased risk of dementia.
Professor Aimee Spector of UCL Division of Psychology and Language Sciences, co-author on the paper, said: “Cognitive symptoms such as forgetfulness and ‘brain fog’ are incredibly common during menopause, yet they are often overlooked. Our findings highlight just how complex menopause-related cognitive symptoms are, and how much we still don’t know about what drives them. More targeted research is essential if we are to identify which biological, psychological or lifestyle factors contribute most, and what types of support or treatment are likely to be effective.”
The authors argue that clinicians can play a key role in understanding and validating women’s experiences by asking about the duration of cognitive symptoms, impacts on day-to-day functioning and any other medical or psychosocial factors that could be contributing to cognitive symptoms.
The review also discusses a range of approaches that may ease cognitive symptoms, such as improving sleep quality, engaging in regular aerobic exercise and eating a balanced diet. There is also little but promising research into the impact of psychological therapies targeting cognitive symptoms, with a recent meta-analysis of three cognitive behavioural therapy-based studies showing significant improvements in memory and concentration. The evidence is more mixed for the benefits of hormone therapy on cognitive symptoms during menopause.
The authors identify cognitive symptoms as a major area of unmet need in menopause research. They call for a unified definition of menopause-related cognitive changes and for prospective, longitudinal studies that can track women from pre- to post-menopause. Better understanding of the biological, psychological and social factors that contribute to cognitive symptoms will be crucial for developing effective treatments.
Lead researcher Dr Caroline Gurvich of Monash University said: “There’s a lot of pressure to use objective measures of cognitive decline, like a memory test, for example, in a clinical trial, but the key symptom of brain fog is a subjective experience. So having a definition that acknowledges the key cognitive symptom is critical.”
This is not without precedent – we already use subjective or self-report measures for depression, anxiety and other mental health conditions with great success.
Dr Gurvich said the proposed definition would also validate women’s individual experiences while empowering them through the reassurance that any objective decline in their cognitive ability is subtle.
She added: “This is a decrease in cognitive or learning efficiency, not functionality or capacity. For many women, the perception they are losing capacity is what drives them to stop work or lose the confidence to live fulfilling lives during and after menopause. I hear all the time from women who have gone through menopause that validation would have made a significant difference to their resilience and the approach they took to living with menopause.”
Co-author Professor Martha Hickey of the University of Melbourne and Royal Women’s Hospital said: “Our analysis of the best available research shows that many women experience some degree of cognitive symptoms, such as brain fog, during the menopause transition.”
“But there’s a lack of long-term data, which means that there’s a gap in our knowledge about how the brain fog symptom develops and changes from peri-menopause to after menopause ends. It’s a real gap in our understanding.”
Professor Spector added: “We increasingly see women, typically at the peak of their careers, losing confidence in the workplace, often translating to leaving work or reducing work hours. Having simple strategies to support and retain them at work is also a broader economic issue.”
Menopause
New Women’s Employment Ambassador role targets workplace health
News
Cooling bracelet targets menopause hot flushes

 Entrepreneur2 weeks ago
Entrepreneur2 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Fertility4 weeks ago
Fertility4 weeks agoMenstruation costs £20,359 a lifetime, sparking calls for Government action

 Menopause4 weeks ago
Menopause4 weeks agoCalifornia plans US$3.4m menopause care overhaul

 Menopause3 weeks ago
Menopause3 weeks agoWatchdog bans five ads for women’s heath claims

 Pregnancy2 weeks ago
Pregnancy2 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Fertility4 weeks ago
Fertility4 weeks agoPeers push to pardon women criminalised under abortion laws

 Menopause3 weeks ago
Menopause3 weeks agoMenopause has no lasting impact on cognition, research finds

 News2 weeks ago
News2 weeks agoTwo weeks left to make your mark in women’s cardiovascular health



























Pingback: 7 Natural Menopause Treatments That Really Work - An TV News
Pingback: 7 Natural Menopause Treatments That Really Work: Effective Remedies - An TV News