News
Common IVF add-on may be ‘a waste of time’, says study
A common IVF add-on could prove an expensive waste of time, researchers have said
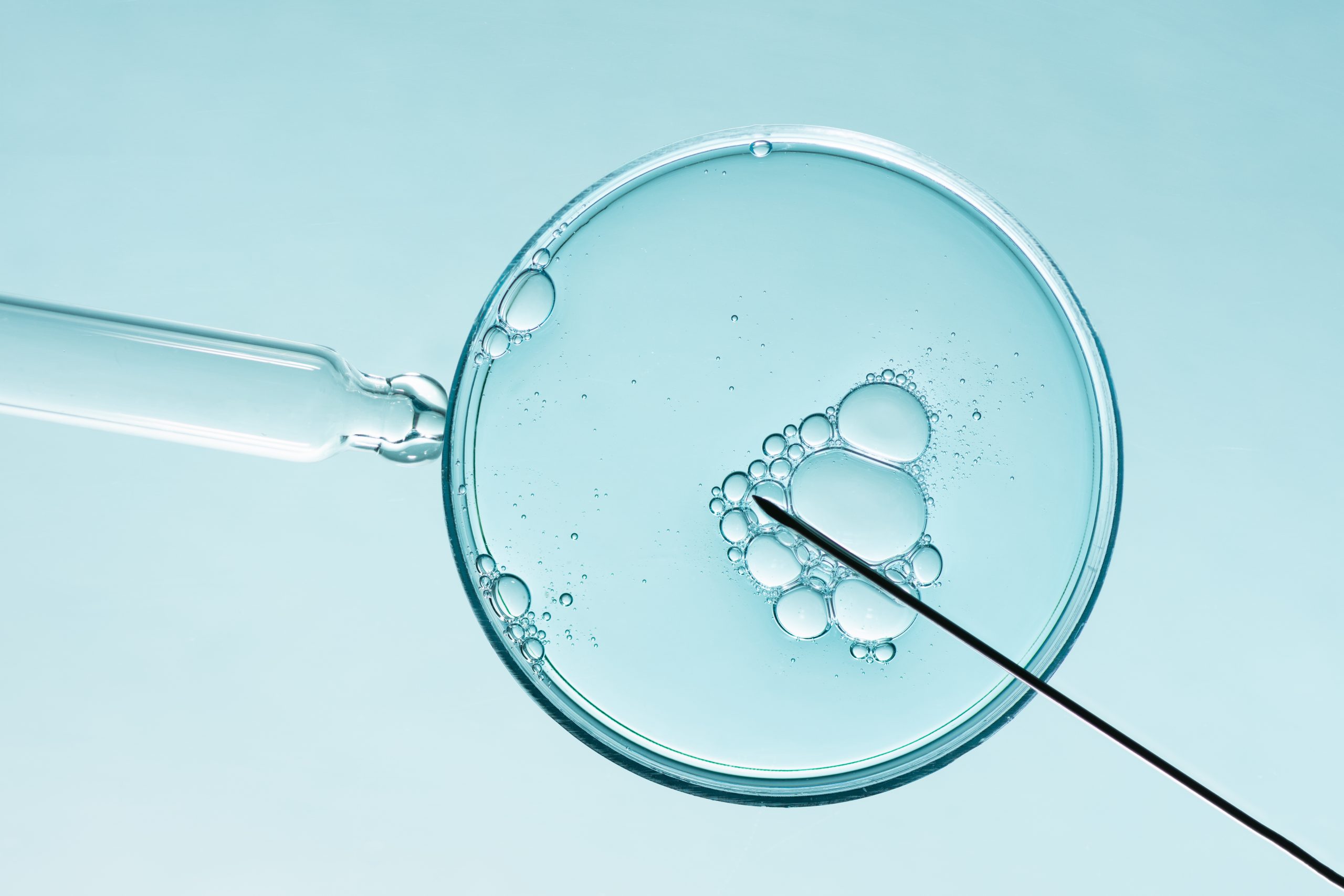
One of the most common IVF add-ons undertaken globally could be a “waste of time”, a new study has found.
The research, conducted by Monash University’s Professor Ben Mol in Australia and Dr Rui Wang and colleagues in China, found that intracytoplasmic sperm injection (ICSI), whereby a single sperm is injected directly into a mature egg, could be an expensive waste of time, in some cases even reducing the chances of success.
Originally developed in 1992 for couples with severe male infertility, ICSI has since expanded in use in more than half of all embryo transfers in Australia and elsewhere.
Over the past 30 years, use of ICSI has increased and now accounts for nearly two thirds of IVF cycles worldwide, including 70 per cent in Europe and North America and nearly 100 per cent in some low-income and middle-income countries.
In 2021, over 100,000 IVF cycles were performed in Australia and New Zealand resulting in the birth of 20,690 babies, a record high for IVF medical treatments.
The proportion of embryo transfer cycles that used embryos fertilised using ICSI was 55.6 per cent in 2021. However, according to Professor Ben Mol, severe male infertility only impacts 30 per cent of couples.
“The use of ICSI far outweighs its original purpose and has been adopted as a general IVF procedures in Australia and globally,” he said.
Mol’s study, published in The Lancet, looked at ten reproductive medicine centres across China. Couples with infertility with non-severe male factor without a history of poor fertilisation were randomly assigned to undergo either ICSI or conventional IVF. The primary outcome was live birth after first embryo transfer.
For a three-and-a-half year period from 2018 to 2021, 2,387 couples were randomly assigned to the ICSI group and the remainder to the conventional IVF group.
Live birth after first embryo transfer occurred in 34 per cent couples in the ICSI group and in 37 per cent of couples in the conventional IVF group.
Looking at the total number of babies born from the started cycle taking into account multiple transfers, this difference increased to 45 per cent after ICSI versus 51 per cent after IVF.
The study, Mol said, showed that in couples with infertility with non-severe male factor, ICSI did not improve live birth rate compared with conventional IVF.
“Given that ICSI is an invasive procedure associated with additional costs and potential increased risks to offspring health, routine use is not recommended in this population,” he said.
He added: “The increased use of ICSI in couples with infertility without severe male factor has boomed because of the belief that use of ICSI might increase fertilisation success, and now we have shown that this is incorrect.”
There are also concerns about ICSI – an invasive procedure that bypasses natural selection barriers during the fertilisation process. A recent Australian study indicated a small increased risk for genitourinary abnormalities after ART, particularly after ICSI.
Professor Mol said: “Because a single sperm is isolated and injected into the egg, the natural selection process where a sperm cell beats millions of competitors is bypassed, which may lead concerns re potential risks to offspring health, including congenital anomalies.”
To receive the Femtech World newsletter, sign up here.
Fertility
Infertility may be risk factor for early menopause, study suggests
pain conditions
Endometriosis documentary profiles stars including Marilyn Monroe and Amy Schumer

A non-profit has launched an endometriosis documentary featuring Amy Schumer and Marilyn Monroe as it pushes for changes in how the condition is treated and understood.
The Endometriosis Collective has launched to change how endometriosis is researched, treated and understood, starting with a documentary featuring stories from people including Amy Schumer and Marilyn Monroe.
The feature-length documentary, “End of the Cycle”, will premiere in New York on Tuesday, and The Endometriosis Collective is making the film free to stream online.
Schumer, a comedian, writer and actor, has previously spoken of how endometriosis left her “on the floor in pain, vomiting from the pain, the pain that nobody can see.”
Schumer is one of several celebrities featured in the documentary. Other contributors include dancer Julianne Hough, Olympic medallist Brittany Brown and actors Janel Parrish and Folake Olowofoyeku.
The Endometriosis Collective timed the documentary premiere to coincide with the 100th anniversary of Marilyn Monroe’s birth.
Monroe, who died in 1962, starred in films such as “Some Like It Hot” and “Gentlemen Prefer Blondes.”
According to a biography published in 1985, Monroe’s endometriosis was so severe that it destroyed her marriages, her wish for children, her career and ultimately her life.
The Endometriosis Collective said the documentary shares newly uncovered information about Monroe’s experience with endometriosis.
The non-profit said the information connects Monroe’s story to the experiences of women across generations, highlighting how far awareness, research and care still have to go.
A representative of the Marilyn Monroe Estate said: “By sharing this part of her story through ‘End of the Cycle,’ we hope to honour her legacy in a way that brings visibility to endometriosis, encourages more open dialogue and helps inspire the research needed to create change.”
As part of the premiere, The Endometriosis Collective is holding a panel discussion.
Schumer, Brown and Olowofoyeku, the documentary’s co-directors Sammy Jaye and Soraya Simi, and medical experts are due to be part of the premiere.
AbbVie’s Orilissa and Sumitomo Pharma’s Myfembree are among the approved drugs for endometriosis pain.
Hough, one of the participants in the documentary, starred in an Orilissa campaign in 2017.
News
Bridging the metabolic wealth gap: The telehealth platform bypassing insurance to democratise care

As weight-loss treatments remain locked behind prohibitive paywalls, a new direct-pay initiative is cutting costs in half for low-income patients, and it could provide a new blueprint for health equity.
It is one of the most persistent, frustrating paradoxes in modern healthcare: the medical innovations most capable of addressing widespread chronic conditions are overwhelmingly priced out of reach for the populations most vulnerable to them.
Nowhere is this more evident than in the current landscape of metabolic health and weight management.
As state governments and insurance providers increasingly restrict coverage for advanced weight-loss medications due to skyrocketing costs, a stark dividing line has emerged. Clinical need is no longer the primary factor in who receives treatment. Affordability is.
This financial barrier disproportionately impacts women, who not only face high rates of metabolic conditions but also frequently serve as the primary caregivers in their households.
For a single mother managing childcare, grueling work hours, and the relentlessly rising cost of living, personal well-being is often the first casualty of a tight budget.
These patients are forced into a holding pattern, watching their conditions progress year after year while highly effective, life-changing treatments remain separated from them by a paywall.
Now, a telehealth platform called Amble Health is attempting to dismantle that wall by bypassing the traditional insurance apparatus entirely.
A Structural Shift for Access
Today, Amble Health announced the launch of the Amble Cares Program, a national initiative designed to cut the cost of medical weight-loss treatments in half for low-income Americans.
The programme arrives at a critical inflection point.
Today, roughly one in eight U.S. adults have utilized advanced metabolic medications, according to a recent KFF Health Tracking Poll.
This surge in adoption has driven a fundamental shift in preventative care, but the distribution of that care has been deeply uneven.
Through the Amble Cares Program, eligible patients can access comprehensive medical weight-loss programmes, which may include prescription medications if clinically appropriate, at up to 50 per cent below standard rates.
To ensure the discounts reach the intended demographic, eligibility is determined by an independent, third-party verification partner, based on verified financial need.
The programme explicitly prioritises individuals and families with limited disposable income, including parents and guardians whose financial flexibility is tied up in providing for dependents.
Once verified, patients are connected directly to licensed clinicians to begin treatment immediately, stripping away the friction of waiting periods.
“Healthcare should not be a luxury item,” said Joey Stiver, CEO of Amble Health. At Amble, we believe that a patient’s zip code or income shouldn’t dictate their metabolic health outcomes.
“The Amble Cares Program is our direct response to the cost of living crisis, moving beyond talk of ‘affordability’ to actually delivering it to the people the traditional system has left behind.”
The Direct-Pay Trade-Off
However, this rapid, lower-cost access comes with a significant structural trade-off.
To achieve these price reductions and eliminate the administrative delays, denials, and red tape associated with traditional healthcare, Amble Health operates strictly as a direct-pay platform.
This means participants cannot use outside coverage. The programme does not accept Medicaid, Medicare, commercial insurance, or even HSA/FSA funds.
For some patients, being entirely locked out of utilizing their existing health benefits may present a new kind of hurdle.
But for those who have already found themselves abandoned by traditional coverage networks, facing outright denials, unnavigable prior authorisations, or insurmountable deductibles, the direct-pay model offers a predictable, transparent alternative to a broken system.
Ultimately, the Amble Cares Program is making a bold bet: that the most efficient way to deliver equitable healthcare to disenfranchised populations isn’t to fix the traditional insurance system, but to innovate entirely around it.

 Menopause1 week ago
Menopause1 week agoPerimenopause misinformation ‘putting women at risk’

 Opinion4 weeks ago
Opinion4 weeks agoWhat Maternal Mental Health Month reveals about where postpartum support actually breaks down

 News4 weeks ago
News4 weeks agoNIH Grant terminations disproportionately impact minority scientists, research finds

 Events4 weeks ago
Events4 weeks agoWUKA brings Period-Positive Pool Party to London Aquatics Centre to keep girls swimming through puberty

 Insight3 weeks ago
Insight3 weeks agoPCOS renamed after decade-long campaign to end ‘cyst’ misconception

 Events4 weeks ago
Events4 weeks agoWHIS 2026 unveils agenda and first speakers for the leading women’s health summit

 Menopause4 weeks ago
Menopause4 weeks agoCBT shows promise for menopause insomnia and hot flashes

 Hormonal health2 weeks ago
Hormonal health2 weeks agoNHS urged to update website following renaming of PCOS


























1 Comment