Wellness
Millennial women are missing lifesaving cancer checks – how to close the cervical screening gap

As new European research shows millennials are more likely to miss cervical cancer screenings than any other generation, experts warn that failing to address major barriers – from fear to family and workplace pressures – could undermine global elimination targets.
Results from a survey of over 5,500 women aged 16-64 found that 31 per cent of eligible millennials have postponed or missed their cervical screening appointments, a figure that is 27 per cent higher than the average across all age groups.
The research, commissioned by Roche Diagnostics and conducted by GWI across six European countries, also found that, despite screening services being widely available free of charge or heavily subsidised in many countries, specific challenges make accessing routine cervical screening difficult for some.
Fears related to pain, embarrassment or stigma surrounding cervical screenings are well-documented as contributing to lower screening rates. But the research also reveals particular challenges millennials face in balancing careers, caregiving responsibilities, and relationships often result in appointments being missed or delayed at a higher rate compared to other age groups.
The ‘have it all’ generation?
“Millennials are often said to be the ‘have it all generation,’ juggling careers, caregiving, and societal expectations. Yet, they tend to put themselves last,” said Joanna Sickler, Vice-President, Health Policy and External Affairs at Roche Diagnostics.
“The research shows that millennials are disproportionately failing to prioritise cervical screening because of a mix of emotional, logistical, and societal pressures.”
Cervical cancer affects more than 600,000 women globally every year, yet it is preventable in almost all cases through vaccination, early detection, and treatment of precancers. Cervical screenings remain vital for detecting human papillomavirus (HPV), the cause of over 99 per cent of cervical cancers, but participation has declined in recent years.
In England, cervical screening rates have fallen to around 69 per cent for women aged 25–64 – well below the NHS England target of 80 per cent – with rates lower for younger women (66 per cent) than older women (74 per cent). According to NHS data, this means over five million women are not up to date with their routine check-up.
The high prevalence of millennials missing screening appointments is particularly concerning, given that they may be the age group that is most at risk. Between 1990 and 2019, cases of early-onset cancer among people under 50 increased by 79 per cent worldwide, and mortality by 28 per cent, making millennials the first generation at greater risk of developing tumours than their parents.
Research also indicates a rise in cases of cervical cancer among millennial women, despite the World Health Organization’s commitment to eliminating it as a public health problem by 2030. A study published in JAMA in 2022 revealed that the incidence of the disease has risen by an average of 2.5 per cent per year among women 30 to 34 years old since 2012.
Experts believe that the reduction in screening uptake among this age group could be contributing to the rise in cervical cancer rates.
A separate study, published in JAMA Network Open, found that of over 20,000 US women surveyed between 2005 and 2019, the percentage of those overdue for cervical cancer screening rose from 14 per cent in 2005 to 23 per cent in 2019.
Women aged 21–29 were significantly more likely to be overdue for screening than those between the ages of 30 and 65.
Fear remains the biggest barrier
According to Roche’s research, fear remains the biggest barrier to attending cervical screenings, with 30 per cent citing fear as the primary reason for missing or delaying their appointments, driven by anxiety about discomfort, pain, or the potential results. This was particularly common among younger generations.
In Spain, 43 per cent of respondents cited fear as a reason for delay, the highest across all surveyed markets. Across the wider survey, 36 per cent of those aged between 16 and 34 years old and 37 per cent of those without children were also significantly more likely to delay due to fear.
This appears to be compounded by a lack of awareness and open dialogue about cervical screening. Despite various public health initiatives to encourage uptake, nearly 50 per cent of respondents, including 43 per cent of millennials, admitted they had never spoken to anyone about cervical screening, with 10 per cent saying they would be more likely to attend if encouraged by family, friends, or colleagues.
“It’s important to create an environment where discussing cervical screening and women’s health topics is not only accepted but encouraged,” Sickler tells Femtech World.
“This can only happen if these topics become commonplace in homes, workplaces and communities.”
Work, family and societal pressures
But fear is not the only factor.
The survey also found that professional commitments and workplace demands are the second-largest barrier for all participants. High-income earners, or those in the top third of income ranges across markets, are 22 per cent more likely than average to delay appointments, and 27 per cent of this group cite workplace demands as the reason for postponement.
Caregiving responsibilities are also often prioritised over personal health, particularly for parents, with 27 per cent of parents surveyed reporting they had delayed or cancelled cervical screening appointments.
Among millennials who postponed their screenings, 12 per cent identified assistance with travel or childcare as a significant motivator, while 19 per cent said greater workplace flexibility and encouragement from employers would help them prioritise their appointments.
According to Sickler, although 66 per cent of managers agree on the importance of taking an active role in supporting employees to attend screenings, only 14 per cent offer flexibility, and just eight per cent have discussed the topic at work.
At the same time, evidence shows the burden of cervical cancer falls disproportionately on marginalised and underserved communities, with incidence rates of cervical cancer in the UK 65 per cent higher in the most deprived quintile of the population, and approximately 520 cervical cancer cases each year linked to deprivation.
Meeting women where they are
Professor Daniel Kelly OBE, Cardiff University, and co-chair of the HPV and Hep B Action Network at the European Cancer Organisation, says healthcare systems “must evolve to meet women where and how they live”. And more broadly, society and communities should “foster open dialogue” to “normalise cervical health as a shared responsibility”.
Sickler agrees that healthcare systems must adapt to better address some of the barriers facing millennial women through practical and cultural solutions – from strengthening awareness and support to streamlining booking systems and expanding access to alternative screening options like self-sampling.
“The latest findings highlight opportunities to improve screening participation through education, workplace flexibility and access to resources,” she says.
“Whilst millennials are the most likely to miss cervical screening appointments, our research also shows they are also the generation most likely to request alternative screening options (21 per cent) and a more convenient booking process (35 per cent).
“To meet these needs, health systems could expand alternative screening options such as self-collection, which offers privacy and convenience and helps overcome barriers like embarrassment, fear of discomfort, and cultural stigma.
Sickler adds: “Streamlining booking processes, strengthening patient education, and fostering open conversations to normalise cervical health are crucial steps in overcoming key barriers.”
NHS to roll out home HPV testing
In England, where the NHS has promised to eliminate cervical cancer by 2040, more women are expected to be offered home screening kits as part of the cervical screening programme outlined in the recently published 10 Year Plan.
From January 2026, HPV self-sampling kits will be offered to those who have rarely or never attended their cervical screening appointment to allow them to test at home. The programme is specifically aimed at groups consistently missing vital appointments, including younger women, ethnicities facing cultural hurdles, people with disabilities and the LGBT+ community.
The new policy was informed by research carried out by King’s College London in 2021, which provided HPV self-sampling kits to women and people with a cervix who were at least six months overdue for their cervical screening. The YouScreen trial found that offering self-sampling kits could boost the numbers screened in England by about 400,000 each year.
According to Dr Anita Lim, visiting senior research fellow at King’s and chief investigator of the trial, the findings demonstrated that self-sampling could reach people who find it difficult to attend traditional screening, including those from diverse and underserved populations.
“It’s hugely positive to see this now reflected in national policy, helping more people get protected from this highly preventable cancer,” said Lim.
While screening carried out by a clinician is still considered the “gold standard” for HPV testing, experts and leading charities such as Cancer Research UK and The Eve Appeal have welcomed the initiative, saying it will help remove barriers and make cervical screening more accessible. And anyone who tests positive for HPV through self-sampling will be encouraged to attend a clinician-taken follow-up screening test.
“The gold standard way to test for HPV is still a sample taken by a clinician, and this will be suitable for most people,” said Michelle Mitchell, Chief Executive of Cancer Research UK, when the plans were announced back in June.
“But beating cervical cancer means beating it for everyone, and this move helps to bring us closer to that goal.”
A ‘societal movement’ to beat cervical cancer
Improving access to self-screening is one solution, but as Sickler highlights, it’s not the whole solution.
Roche’s new campaign, ‘Cervical cancer: it only ends with all of us’, focuses on several different ways to encourage those eligible to overcome barriers and attend clinician-collected cervical screenings.
This includes promoting more emotional and practical support from loved ones, better education across communities, and open conversations around the topic.
“The campaign aims to improve attendance rates through a societal movement to encourage and empower eligible populations to attend their cervical screening appointments,” Sickler adds.
“Only by creating an inclusive environment where women’s health topics are discussed will we be able to increase attendance and prevent cervical cancer from continuing to claim lives.”
Menopause
New Women’s Employment Ambassador role targets workplace health
Pregnancy
Physicians neglecting preventive care for women with diabetes, study finds
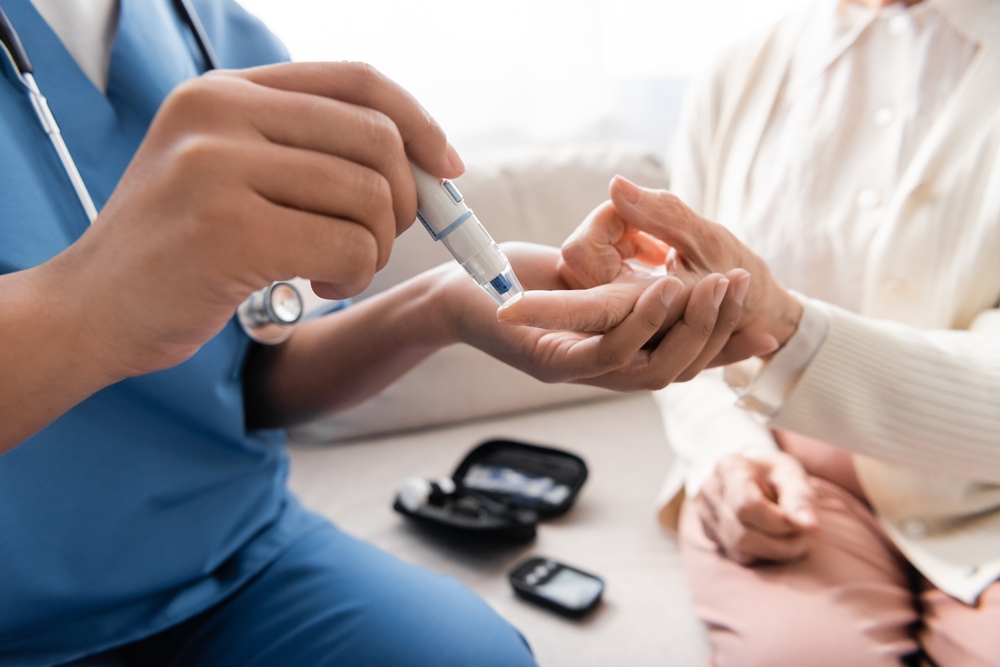
Women with diabetes are less likely to get preventive care than those without the condition, a UCLA-led study suggests.
The findings are based on an analysis of more than 40 studies from several countries.
They highlight how physicians largely overlook the importance of these routine services for women who have diabetes mellitus, or DM, putting them at risk of preventable medical conditions such as pregnancy complications.
Lauren Wisk is associate professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA and senior author on the study.
She said: “These findings are important because they identify that women with diabetes are not receiving recommended well-woman care, which is essential to support both managing their diabetes and their overall health.
“Providers need to be aware that they should not forget to provide these essential services for women with diabetes.”
The researchers sifted through thousands of studies, focusing on the concepts of women, diabetes and women’s health services, and settled on 44 that addressed treatment services for women aged 15 to 49 with type 1 or type 2 diabetes, excluding those with diabetes insipidus or gestational diabetes.
They looked at four preventive health service categories: contraceptive counselling and use, breast and cervical cancer screening, pre-conception counselling, and screening for sexually transmitted infections.
One study found that 48 per cent of women with diabetes received contraceptive services compared with 62 per cent of women without the disease.
Nine papers showed cervical cancer screening rates ranging from 38 to 79 per cent for women with diabetes compared with 46 to 86 per cent for those without diabetes.
Four studies found that breast cancer screening rates for women with diabetes ranged between 38 and 69 per cent compared with 54 and 82 per cent for those without diabetes.
Fourteen studies found pre-conception counselling rates of just over 1 per cent compared with 46 per cent for women with diabetes who are planning to get pregnant.
The researchers did not identify any studies on screening for sexually transmitted infections, which they said represents “a substantial gap in the literature.”
The researchers wrote: “One of the more striking findings of this review is the importance of robust coordinated care teams in ensuring access to appropriate services for women with DM.
“Several of the identified studies provide support that a co-management model, or the concept of involving endocrinology, primary care, and other specialty care providers in the care of individuals with DM, as recommended by the American Diabetes Association, is associated with greater receipt of services.”
Within the time constraints of an office visit, primary care physicians are expected to address preventative health needs as well as chronic disease management, said Dr Lisa Kransdorf, an associate clinical professor of medicine at the Geffen School and a study co-author.
She said chronic disease management will often take priority.
“In cases where the patient has other providers such as specialists and clinical pharmacists actively involved in their chronic disease management, there is opportunity for primary care physicians to attend to preventative care gaps,” the researcher added:
There are some limitations to the findings.
The search yielded only 44 studies, many of which relied on patient recall, which can be unreliable, highlighting the need for further research.
In addition, most of the studies analysed had small sample sizes or were conducted at a single site, limiting how applicable the findings might be in other settings.
News
WUKA’s Tackle Anything campaign reaches 6,000 Girls

WUKA’s Tackle Anything campaign has officially reached their goal of supporting 6,000 girls across grassroots sports clubs in the UK – making a major milestone in the fight to keep girls in sport.
WUKA believes no girl should have to stop playing because of her period.
Yet for many young athletes, that’s still the reality. Fear of leaking through kit, managing cramps during training, or lacking access to sustainable period products continues to push girls out of sport.
The scale of the issue is impossible to ignore:
- 3 in 4 girls avoid sport and physical activity during their period
- This figure rises to 78 per cent among girls who have dropped out of sports.
- 43 per cent of girls drop out of sport after primary school
Source: https://womeninsport.org
That’s why WUKA, the award-winning, pioneering, female-founded period care brand, launched Tackle Anything – a campaign designed to support girls at grassroots level and create more period-inclusive sports environments from the very start of their journeys.
Since launching, the initiative has supported over 6,000 girls across a wide range of sports, including football, rugby, netball, roller hockey and taekwondo, reaching clubs in England, Scotland and Wales.
Through the campaign, clubs receive free WUKA Teen Stretch period underwear for young athletes, alongside expert-led period education delivered in partnership with 3x Olympian and Commonwealth, Euro & World Champion Hannah Miley MBE.
The programme helps coaches, parents and players feel more confident supporting girls in sport – both physically and emotionally
Continuing the Mission
While reaching 6,000 girls is a huge milestone, WUKA says the work is far from over.
The brand is continuing to expand Tackle Anything, with plans to support even more clubs and reach thousands more girls – ensuring that periods are no longer a barrier to participation in sport.
Because staying in the game shouldn’t depend on your cycle.
Founder and CEO of WUKA, Ruby Raut says: “At WUKA, this has never been about visibility – it’s about freedom.
“Freedom for girls to show up, play, and stay in sport without their period holding them back. Reaching 6,000 girls is a huge milestone, but for us, it’s part of a much bigger fight.
“We’ve already helped change the game, and we’re committed to continuing that progress.
“Every time we hit a goal, we set a new one — because this isn’t the finish line. It’s about shaping the future of sport and making sure the next generation grows up feeling confident, supported, and unstoppable.
Dean Wigzell (Head of Community Engagement at Kings Langley FC) adds: “The club is proud to be working with WUKA.
“Partnerships like this further reinforce our belief that our club is fast becoming the club to be at for young female footballers.”
The WUKA Mission:
WUKA – short for Wake Up Kick Ass – is on a mission to eliminate shame, silence, and stigma around periods.
Their commitment to menstrual equity in sport is starting where it matters most: at the beginning.
Because when you empower girls early, you don’t just keep them in the game – you change the future of the game itself.
Part of a Bigger Fight
This builds on WUKA’s wider activism – including their #AxeTheTax campaign, which successfully removed the tax on period pants, and continues to fight for true menstrual equity in the UK, including in sports.
Because access isn’t a luxury – it’s a right. WUKA is now making sure girls aren’t priced out of the game or made to feel like their period holds them back.
This isn’t just about products – it’s about freedom, fairness, and creating a level playing field for every girl.
To learn more about the campaign or explore how your club or organisation can get involved, visit: https://wuka.co.uk/pages/tackle-anything.

 Entrepreneur2 weeks ago
Entrepreneur2 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Fertility4 weeks ago
Fertility4 weeks agoMenstruation costs £20,359 a lifetime, sparking calls for Government action

 Menopause3 weeks ago
Menopause3 weeks agoCalifornia plans US$3.4m menopause care overhaul

 News4 weeks ago
News4 weeks agoHalogen Ventures surpasses 100 investments in female-founded startups

 Menopause3 weeks ago
Menopause3 weeks agoWatchdog bans five ads for women’s heath claims

 Pregnancy2 weeks ago
Pregnancy2 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Fertility4 weeks ago
Fertility4 weeks agoPeers push to pardon women criminalised under abortion laws

 Mental health3 weeks ago
Mental health3 weeks agoMenopause has no lasting impact on cognition, research finds






























