Insight
Precision oncology is here — So why are so many breast cancer treatments still a gamble?

By OncoGenomX, Allschwil, Switzerland
When it comes to breast cancer treatment, one truth remains painfully clear: despite decades of progress we still cannot answer the question which treatment(s) a tumour will respond to.
At OncoGenomX, we think it’s time to change that.
We now have tools that allow us to look inside a tumour, understand how it behaves, and predict what treatments will work best—not just for a cancer subtype, but for an individual tumour, with its unique biology.
It’s called Precision Oncology, and it’s one of the most promising frontiers in cancer care. But right now, its full potential is still out of reach for too many patients.
So why the gap?
The Promise: Personalised Treatment That Works the First Time
The dream of precision medicine is simple: treat the person, not just the disease.
In breast cancer, doctors already use some personalised tools. For example, hormone receptor tests help decide whether a patient should receive endocrine therapy.
Genetic tests like Oncotype DXTM or MammaprintTM can help determine whether chemotherapy is needed. These are great first steps.
But here’s the problem: these tools don’t go far enough. They often tell us what could work, but not what will work. Many patients are still treated based on probabilities and population averages, not precise predictions tailored to their specific tumour.
The result? Too many women receive therapies that don’t work—or stop working quickly. Some get treatments that are too aggressive. Others don’t get enough.
The Reality: Cancer Is Chaotic
Part of the reason breast cancer is so difficult to treat is that no two tumours are alike. Even within a single tumour, cells can behave very differently.
Scientists call this “coordinated chaos.” It means that a treatment might hit some parts of a tumour—but miss others entirely. It also means that two women with the “same” diagnosis may need completely different treatments.
In one major study, only about 1 in 5 patients with advanced cancer actually received all the treatments they were genetically eligible for. Even more worrying: in half of the cases, at least one drug in the treatment plan was likely ineffective.
This isn’t just a medical issue—it’s an economic one. Unmatched or suboptimal therapies drive up costs, delay results, and cause unnecessary side effects.
Precision isn’t just better for patients—it’s better for health systems too.
The Breakthrough: Predicting Treatment Response
At OncoGenomX, we believe the missing link is prediction.
We need tools that can do more than classify tumours or identify potential drug targets. We need models that predict how a specific tumour will respond to tailor-made treatment combination.
That’s why we created PredictionStar™, a clinical decision-support tool designed to help oncologists choose optimal treatment combinations, earlier.
It works by analysing real patient data, tumour biology, and how different therapies interact—so doctors can plan treatment combinations based on what’s most likely to work in concert.
In hypothesis generation studies, we’ve seen a 15–22 per cent improvement in treatment success rates—especially beyond first-line therapy. And when treatments work better, patients do better: survival improves, side effects decrease, and costs drop.
The Future: Smarter, More Human-Centered Oncology
We’re not claiming to cure cancer. But we do believe that better decisions lead to better outcomes.
Our goal is to help oncologists move away from treatment decisions based on probabilities and population averages towards truly rational and individualised treatment planning. That means:
Understanding which therapies are likely to work before trying them
Combining treatments in ways that maximise long-term benefit
Matching each patient to the right combination—any treatment line
This is especially important for women’s health.
Breast cancer is the most common cancer among women worldwide. Yet many women still receive treatments that don’t reflect the full complexity of their disease—or the sophistication of today’s science.
Why It Matters for FemTech
At its core, precision oncology is a FemTech issue. It’s about using technology, data, and science to improve women’s lives.
Breast cancer doesn’t affect all women equally. Outcomes vary by age, race, income, and geography.
That’s why we must ensure that the tools of precision oncology are accessible, equitable, and informed by real-world data from all patients—not just clinical trial populations.
By combining human data, artificial intelligence, and biology, we can move toward a future where every woman receives the best possible care, from the very first treatment.
A Question Worth Asking
If there were a tool with the potential to help doctors select the right treatment combination for a patient’s tumour—based on predictive information—wouldn’t we want them to use it?
At OncoGenomX, we think the answer is clear.
The future of breast cancer care is personal. Let’s make it predictable, too.
Find out more about OncoGenomX at oncogenomx.ch
News
Condé Nast to close women’s health magazine after 47 years

Condé Nast will close its women’s health publication Self after 47 years, with unprofitable editions of Glamour and Wired also set to shut.
In a memo published on the magazine giant’s website on Thursday, the media company’s chief executive, Roger Lynch, said: “As audience behaviours shift, we have not seen a path for Self to continue in its current form as a digital publication.”
“Going forward, health and wellness content will be integrated into our other brands, including Allure and Glamour,” Lynch said, referring to Condé Nast’s other beauty and wellness titles.
Self, which moved to an online-only format in 2017, still reaches more than 20m people each month.
The publication has also earned significant recognition over the years, including a National Magazine award and a Webby’s People’s Voice award.
The closure is part of a wider set of operational changes across the company. Lynch also announced the end of Wired’s Italy edition, noting that while the brand “remains a strong global brand, the Italian edition has not kept pace with growth in our other markets”.
Condé Nast will also wind down Glamour’s publishing operations in Germany, Spain and Mexico.
Lynch said: “Taken together, Wired in Italy, Self and the affected Glamour markets represent a little over 1 per cent of our overall revenue.
“They also remain unprofitable, and continuing to operate them in their current form limits our ability to invest in the ideas and areas that will drive future growth.”
Beyond editorial changes, the company is also restructuring internally to adapt to technological shifts.
Lynch said Condé Nast would make “changes within our technology organisation, reflecting the rapid advancement of AI and its impact on our ability to innovate and build products faster”, adding: “Teams will be restructured to be more agile and to work more closely with our brands and customers, reducing barriers to execution.”
The latest moves follow a series of transformations at Condé Nast in recent years.
Glamour ended its print edition in 2018, followed by Allure moving to a digital-only format in 2022.
In 2024, music publication Pitchfork was folded into GQ, the company’s men’s style magazine.
More recently, last November, Vogue, one of Condé Nast’s key revenue drivers, announced it would absorb Teen Vogue to create a more “unified reader experience across titles”.
The media industry has been shrinking steadily over the years.
From 2010 to 2017, the industry lost an average of 7,305 jobs annually, according to data from Challenger, Gray & Christmas published in December 2025.
Since 2018, the average number of job cuts in the industry has risen to 14,298 a year.
Insight
GSK ovarian and womb cancer drug shows promise in early trial
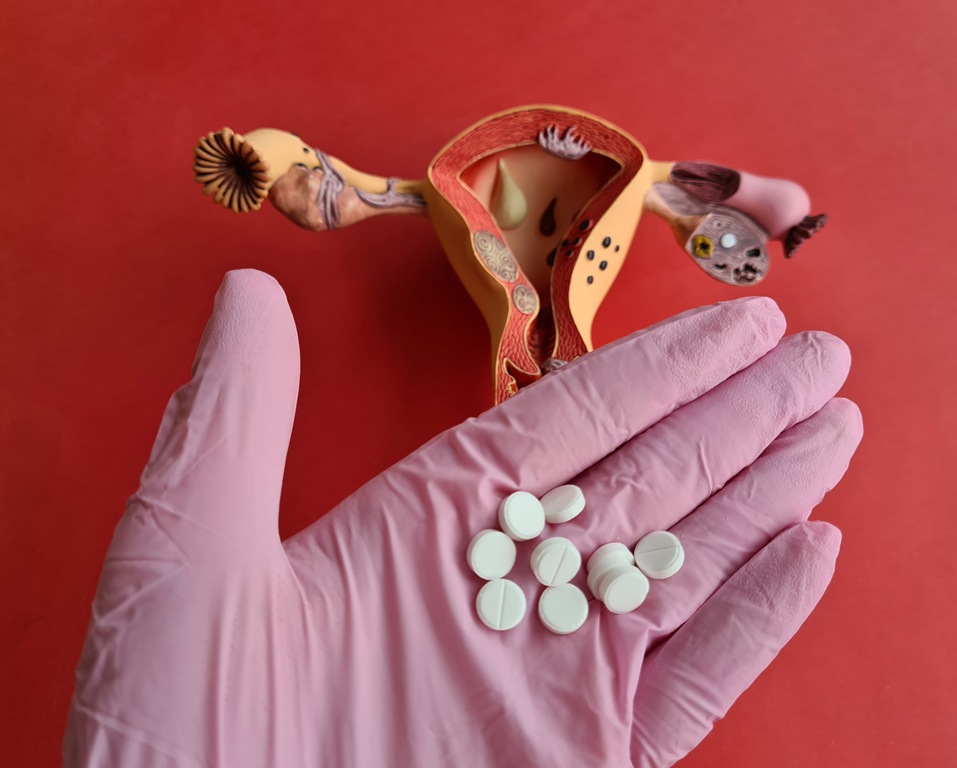
GSK said its ovarian cancer drug shrank or cleared tumours in more than 60 per cent of patients in an early trial as CCO Luke Miels pushes faster development.
The company said that in an early-stage trial, Mocertatug Rezetecan, known as Mo-Rez, shrank or eliminated tumours in 62 per cent of patients with ovarian cancer after chemotherapy had failed, and in 67 per cent of those with endometrial cancer.
Hesham Abdullah, GSK’s global head of cancer research and development, said: “Treatment of gynaecological cancers remains a major challenge, with a pressing need for new therapies that offer improved response rates.
“With Mo-Rez we now have compelling evidence of a promising clinical profile.”
GSK acquired the Mo-Rez treatment, an antibody-drug conjugate, from China’s Hansoh Pharma in late 2023 and has trialled it in 224 patients around the world, including the UK, over the past year.
Only a few patients needed to stop treatment because of side effects, the most common being nausea.
It is given every three weeks by intravenous infusion, meaning directly into a vein.
Combined with data from a separate intermediate trial in China, the results have given the British drugmaker the confidence to go straight to late-stage trials, with five clinical studies planned globally in the next few months, including on patients in the UK.
Speaking to journalists before the conference, Abdullah described Mo-Rez as a “key asset” in the company’s growing cancer portfolio.
It is expected to be a blockbuster drug, with peak annual sales of more than £2bn, which GSK hopes will help it achieve its 2031 sales target of £40bn.
A few years ago GSK did not have any cancer drugs on the market, but it now has four approved medicines and 13 in clinical development.
Last year, oncology generated nearly £2bn in sales, up 43 per cent from 2024, with sales of its endometrial cancer drug Jemperli rising 89 per cent.
News
Self-employment linked to better cardiovascular health outcomes in Hispanic women

Self-employment is linked to lower rates of high blood pressure, obesity, diabetes, poor health and binge drinking in Hispanic women, research suggests.
The findings, published in the peer-reviewed journal Ethnicity & Disease, suggest work structure may be related to cardiovascular disease risk among this group.
Dr Kimberly Narain is assistant professor of medicine in the division of general internal medicine and health services research at the David Geffen School of Medicine at UCLA, senior author of the study, and director of health services and health optimisation research for the Iris Cantor-UCLA Women’s Health Center.
She said: “Hispanic women experience a disproportionate burden of heart disease compared to non-Hispanic women. This is the first study to link the structure of work with risks for heart disease among this group of women.”
The researchers examined 2003 to 2022 data from the Behavioral Risk Factor Surveillance System to assess the association between self-employment, cardiovascular disease risk factors and health outcomes for Hispanic women.
The data included 165,600 Hispanic working women. Of those, about 21,000, or 13 per cent, were self-employed rather than working for wages or a salary.
Overall, the researchers found that self-employed women were less likely to report cardiovascular-disease-associated health problems.
They were also about 11 per cent more likely to report exercising compared with their non-self-employed counterparts.
Specifically, they found that self-employed Hispanic women had a 1.7 percentage point lower chance of reporting diabetes, roughly a 23 per cent decline.
They also had a 3.3 percentage point lower chance of reporting hypertension, roughly a 17 per cent decline.
The study also found a 5.9 percentage point lower chance of reporting obesity, roughly a 15 per cent decline.
It found a 2.0 percentage point lower chance of reporting binge drinking, roughly a 2 per cent decline.
It also found a 2.5 percentage point lower chance of reporting poor or fair overall health, roughly a 13 per cent decline.
The relationship between heart disease risks and the structure of work among Hispanic women was not driven by access to healthcare or differences in income, Narain said.
In fact, the decrease in high blood pressure linked to self-employment was nearly as large as the decrease in high blood pressure linked to being in the highest income group.
The study has some limitations.
The researchers relied on self-reported outcomes, which might be less reliable among ethnic and racial minorities and those from a lower socioeconomic background.
In addition, the researchers’ definition of poor mental health does not entirely match the accepted definition in the fifth edition of the Diagnostic and Statistical Manual of Mental Disorders.
They also did not have data allowing them to examine the specific types of occupations held by the women.
The study design also cannot prove any causal relationship between self-employment and cardiovascular disease risk, which is a subject the researchers will explore.
“The next step in the research is to conduct studies that are able to better assess if the structure of work is a cause of higher heart disease risks among Hispanic women.”
Narain said this.
Study co-authors are Lisette Collins, who led the research, and Dr Frederick Ferguson of UCLA.
Grants from the Iris Cantor-UCLA Women’s Health Center-Leichtman-Levine-TEM program and the UCLA National Clinician Scholars Program supported the research.

 Entrepreneur3 weeks ago
Entrepreneur3 weeks agoThree sessions that show exactly where women’s health is heading in 2026

 Pregnancy3 weeks ago
Pregnancy3 weeks agoHow NIPT has evolved and what AI NIPT means in 2026

 Menopause4 weeks ago
Menopause4 weeks agoWatchdog bans five ads for women’s heath claims

 Entrepreneur4 weeks ago
Entrepreneur4 weeks agoWHIS USA 2026 announces first ticket release for landmark Women’s Health Innovation Summit

 Menopause4 weeks ago
Menopause4 weeks agoMenopause has no lasting impact on cognition, research finds

 News3 weeks ago
News3 weeks agoTwo weeks left to make your mark in women’s cardiovascular health

 Opinion3 weeks ago
Opinion3 weeks agoQ1 momentum: Female founders are advancing, but the system still hasn’t caught up

 News4 weeks ago
News4 weeks agoEndometriosis firm wins NIH prize


























4 Comments