Cancer
Trastuzumab emtansine improves long-term survival in HER2 breast cancer
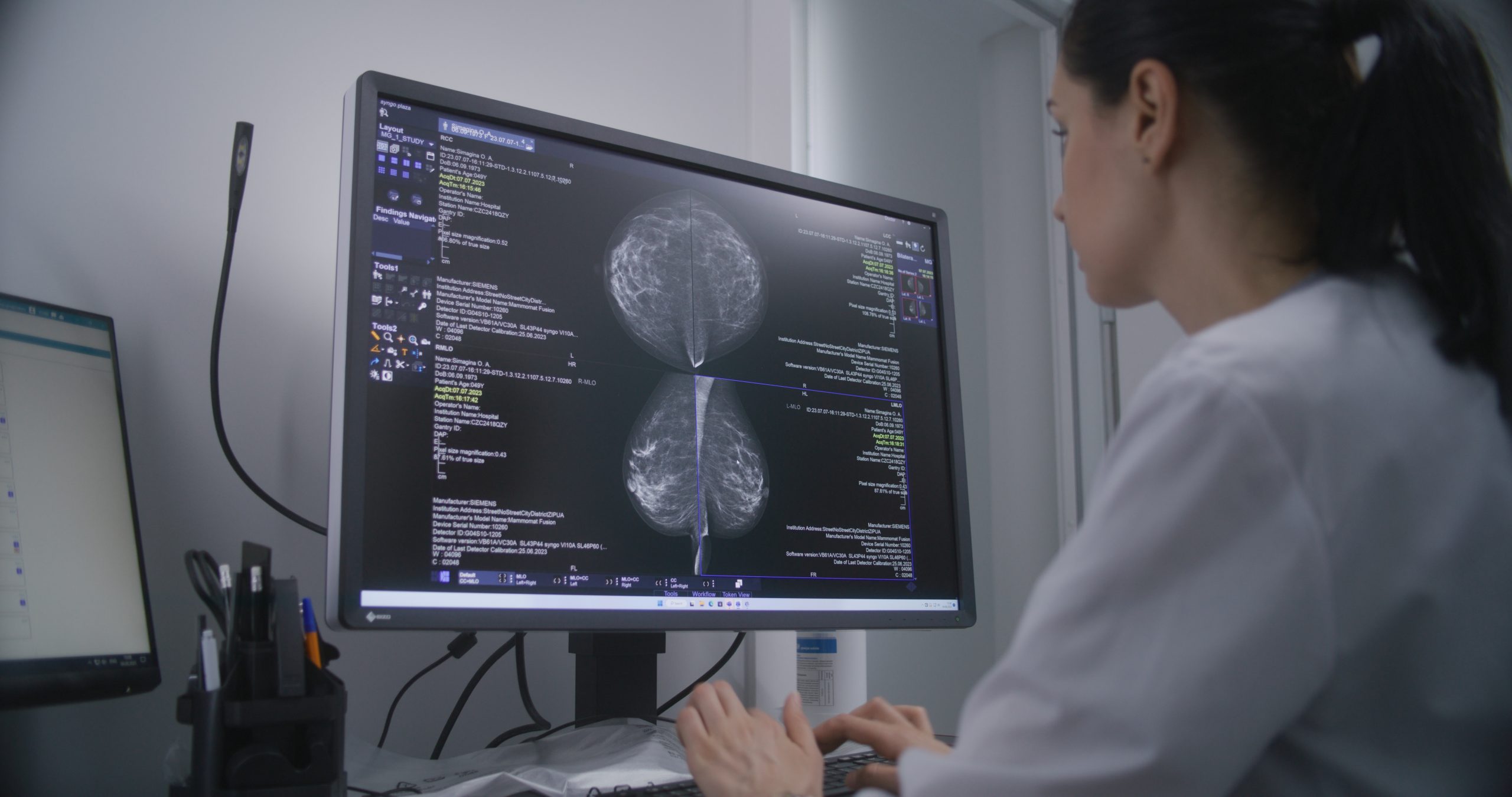
A clinical trial has found that, in patients with high-risk HER2-positive breast cancer, post-surgery, or adjuvant, treatment with trastuzumab emtansine (T-DM1) reduced the long-term risk of death or invasive disease by 46 per cent and improved survival compared to trastuzumab alone.
The findings provide long-term evidence that T-DM1 is an effective adjuvant treatment for this population of breast cancer patients, supporting initial results with three-year follow-up published in the NEJM in 2019, which found that TDM1 reduced the risk of death or invasive disease by 50 per cent.
“KATHERINE is a landmark clinical trial that found T-DM1 had such improved activity relative to trastuzumab that the results were reported earlier than had been anticipated when the study was originally designed. The results changed the standard of care globally for patients with HER2-positive early breast cancer,” said lead author Charles Geyer Jr., professor in the Division of Malignant Hematology and Medical Oncology at the Pitt School of Medicine, UPMC Hillman and UPMC Magee-Womens Hospital.
“We continued to follow patients to understand the full magnitude of the benefit, and we now show that T-DM1 leads to stable long-term improvements in invasive disease-free survival and improves overall survival.”
T-DM1 is an antibody-drug conjugate that combines trastuzumab and a chemotherapy drug called emtansine. When trastuzumab attaches to the HER2 receptor on cancer cells, it acts like a trojan horse, allowing emtansine to more effectively enter the cancer cells and kill them from within.
The KATHERINE trial included 1,486 patients with human epidermal growth factor receptor 2 (HER2)-positive early breast cancer who had residual invasive disease in the breast or axillary lymph node after pre-surgery, or neoadjuvant, treatment with taxane-based chemotherapy and the HER2-targeted agent trastuzumab and surgical removal of the tumour.
These patients are at high risk of cancer recurrence and death.
After surgery, patients were randomly assigned to receive adjuvant standard trastuzumab or T-DM1.
At 7-years follow up, invasive disease-free survival was 80.8 per cent with adjuvant T-DM1 and 67.1 per cent with adjuvant trastuzumab alone. Overall survival was 89.1 per cent with T-DM1 and 84.4 per cent with trastuzumab alone.
Although adverse events were higher in the T-DM1 group (26.1 per cent) compared to patients who received trastuzumab (15.7 per cent), the overall safety of the drug was considered acceptable.
According to Geyer, an important finding was the consistent benefit of T-DM1 across patient subgroups. The analysis showed an approximately 50 per cent reduction in risk of death and invasive disease regardless of the extent of disease at presentation, hormone receptor status, neoadjuvant treatment regimen, pathological node status at surgery, age and race.
“When I started my career in oncology, we knew that some breast cancers were more aggressive, but we didn’t know why,” said Geyer.
“From the excitement of identifying HER2 gene amplification and resultant protein overexpression as a targetable oncogene, through the development of drugs targeting HER2 amplification and evaluating them in landmark clinical trials, I’ve had the privilege of being part of the HER2 story, and it’s incredibly satisfying to have been part of research effort that has led to a new standard of care for patients with this disease.”
Now, Geyer and his colleagues are investigating a promising new antibody-drug candidate called trastuzumab deruxtecan, or T-DXd, for certain groups of patients such as those with lower expression levels of the HER2 protein who didn’t respond as well to T-DM1 as patients with high HER2 expression.
“As oncologists, we are greedy,” said Geyer. “We will never be satisfied until we reach 100 per cent cancer-free survival outcomes for our breast cancer patients.”
Diagnosis
FDA delays ruling on ‘game-changer’ breast cancer drug

The FDA has delayed approval of camizestrant while it reviews new analyses submitted by AstraZeneca after advisers voted against the breast cancer drug.
The US regulator had been considering whether to approve the oral treatment after a phase 3 switching study in a specific group of breast cancer patients.
Camizestrant is an oral SERD, or selective oestrogen receptor degrader. These drugs are designed to block and break down oestrogen receptors that can help some breast cancers grow.
AstraZeneca filed for approval based on the phase 3 Serena-6 trial, which tested a treatment-switching approach.
Patients in the study received an aromatase inhibitor and a CDK4/6 inhibitor. Aromatase inhibitors lower oestrogen levels, while CDK4/6 inhibitors are targeted cancer drugs that help slow cancer cell growth.
After detecting an ESR1 mutation, investigators switched the aromatase inhibitor to camizestrant.
An ESR1 mutation is a change in a gene linked to the oestrogen receptor. It can make some breast cancers less responsive to standard hormone treatments.
AstraZeneca said switching to camizestrant was linked to a 56 per cent increase in progression-free survival.
Progression-free survival measures how long a patient lives without their disease getting worse.
However, the FDA raised questions about the study design.
An FDA advisory committee later voted six to three that AstraZeneca had failed to show camizestrant provides a clinically meaningful benefit.
The vote was a setback for the company’s hopes of approval, although the FDA can go against advisory committee recommendations.
After the setback, AstraZeneca submitted additional analyses requested by the FDA.
The company said the analyses include data on circulating tumour DNA clearance linked to longer-term efficacy outcomes.
Circulating tumour DNA refers to fragments of genetic material from cancer cells that can be found in the blood.
AstraZeneca is expected to share the data next week at the American Society of Clinical Oncology annual meeting.
The FDA has now delayed its ruling while it reviews the additional information. AstraZeneca did not provide a new decision date.
Three-month delays are typical and, during the second Trump administration, have been common.
After budget cuts reduced its workforce, the FDA delayed rulings on assets including Bayer’s Lynkuet, Biohaven’s troriluzole and Sanofi’s tolebrutinib. The FDA reportedly blamed a “heavy workload and limited resources” for one delay.
The agency has continued to delay rulings this year, with Biogen, Savara and Travere Therapeutics among the companies to say the FDA has extended reviews of their drugs.
Like AstraZeneca, those three companies faced delays after submitting additional information that the agency needed time to review.
If the additional analyses address the regulator’s concerns, AstraZeneca could still secure approval for a drug it has estimated could generate peak sales of more than US$5bn.
Guggenheim Securities analysts recently described the Serena-6 study as “a limited commercial opportunity in our and [AstraZeneca’s] view”.
AstraZeneca is also running two adjuvant studies and a trial in a first-line setting as it seeks to position camizestrant across different stages of breast cancer care.
Adjuvant treatment is given after primary treatment, such as surgery, to reduce the risk of cancer returning. First-line treatment is the first therapy given for a disease.
Roche reported the failure of its rival oral SERD in first-line breast cancer in March, but AstraZeneca executives have argued that their trial designs and drug candidate are different.
Last week, Europe’s Committee for Medicinal Products for Human Use issued a positive opinion on camizestrant.
The drug is expected to be marketed as Etcamah in Europe.
Cancer
Early PET scan could chemo response in aggressive breast cancer – study
Diagnosis
Women unaware of gynaecological cancers

Only one per cent of women can name all five gynaecological cancers, new research suggests, as 21 women in the UK die every day of the diseases.
The report also found that 31 per cent of women have put off or avoided seeking medical advice for gynaecological symptoms.
It also found that 43 per cent of women invited for cervical screening said barriers had put them off attending, while 18 per cent of respondents aged 25 to 34 who had been invited had never attended.
The five main gynaecological cancers are womb, also called uterine, ovarian, cervical, vulval and vaginal cancer.
The Lady Garden Foundation said that, while progress has been made since the UK government’s 2022 Women’s Health Strategy aimed to improve gynaecological cancer care, significant challenges remain.
John Butler, medical director and trustee at the Lady Garden Foundation, said: “The fact that only one per cent of the population can name the diseases that directly affect half of us underscores a significant awareness gap, impacting individuals’ ability to recognise vital signs and symptoms or seek timely medical help.
“Addressing this isn’t just about awareness; it’s a critical public health priority. Our collective efforts are essential to ensure the latest commitments announced by this government translate into tangible change that saves lives.”
The report said key reasons for delaying medical advice included difficulty making appointments, embarrassment and, for cervical screening, fear of pain or previous bad experiences.
Women also reported challenges within healthcare interactions, including feeling “not taken seriously”, “dismissed” or “not believed” when seeking gynaecological advice.
Jenny Halpern Prince, chief executive and charity co-founder, said: “We frequently hear reports of women feeling ‘not taken seriously,’ ‘dismissed,’ or ‘not believed’ when seeking gynaecological advice.
“These experiences highlight crucial areas where we can improve patient support and trust within our healthcare system, ensuring women receive the empathetic and effective care they need.”
The Lady Garden Foundation said it aims to increase awareness of both the charity and the five gynaecological cancers.
It also aims to serve as a primary entry point for reliable, stigma-free information, helping people understand their bodies, recognise symptoms and overcome barriers to accessing care.
Its Silent No More Garden was unveiled at the RHS Chelsea Flower Show 2026. Designed by Darren Hawkes, the garden serves as a national call to action, using five sculptures to spark conversations, break long-standing taboos and encourage open dialogue about symptoms and preventative care.
Butler said: “Continued focus and collaborative action are essential to progress.
“The ongoing commitment from the government, alongside societal efforts to break down taboos surrounding gynaecological health, are crucial.
“The Lady Garden Foundation is dedicated to being a beacon of information and support, empowering women with the knowledge they need. We urge everyone to learn the signs, speak up, and help us save lives.”

 Motherhood4 weeks ago
Motherhood4 weeks agoWhat Maternal Mental Health Month reveals about where postpartum support actually breaks down

 News3 weeks ago
News3 weeks agoNIH Grant terminations disproportionately impact minority scientists, research finds

 Menopause5 days ago
Menopause5 days agoPerimenopause misinformation ‘putting women at risk’

 Adolescent health3 weeks ago
Adolescent health3 weeks agoWUKA brings Period-Positive Pool Party to London Aquatics Centre to keep girls swimming through puberty

 Insight3 weeks ago
Insight3 weeks agoPCOS renamed after decade-long campaign to end ‘cyst’ misconception

 Events4 weeks ago
Events4 weeks agoWHIS 2026 unveils agenda and first speakers for the leading women’s health summit

 Menopause3 weeks ago
Menopause3 weeks agoCBT shows promise for menopause insomnia and hot flashes

 Insight4 weeks ago
Insight4 weeks agoOnline abuse and deepfakes ‘pushing women out of public life’



























